


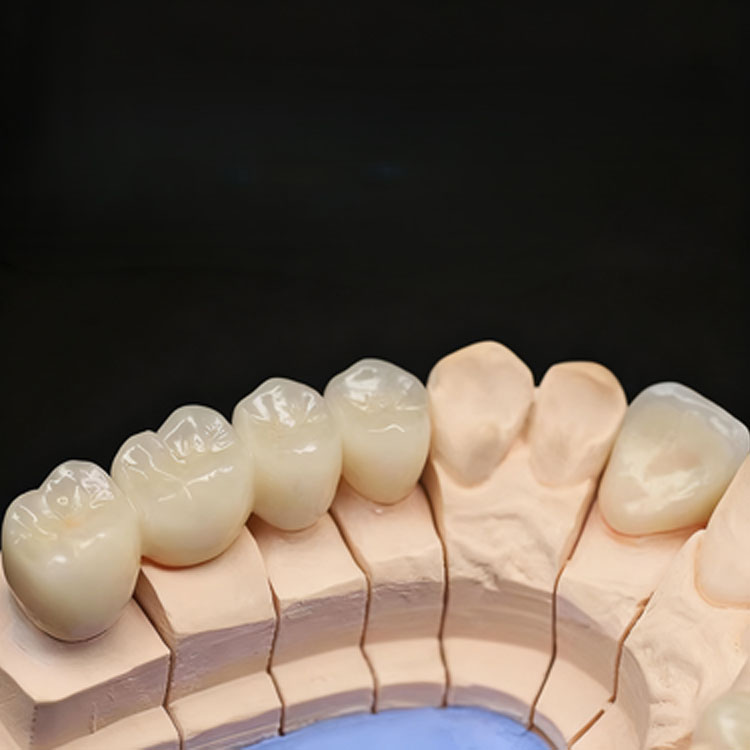
Большинство клиницистов рассматривают это как вопрос эстетики. Я так не считаю. Реальная грань между винирами E.max и коронками E.max в первую очередь биологическая, во вторую - механическая, и только потом - косметическая.
Сначала три слова.
Хватит гадать.
Я видел слишком много косметических случаев, которые продавались как “виниры”, когда препарирование, картина трещин, старая композитная карта и окклюзия уже кричали о “коронке”, и именно так хорошие планы лечения превращаются в чувствительность, дебонды, переделки и ту тишину в кабинете, которая никому не нравится. Почему мы продолжаем вести себя так, будто это выбор стиля?
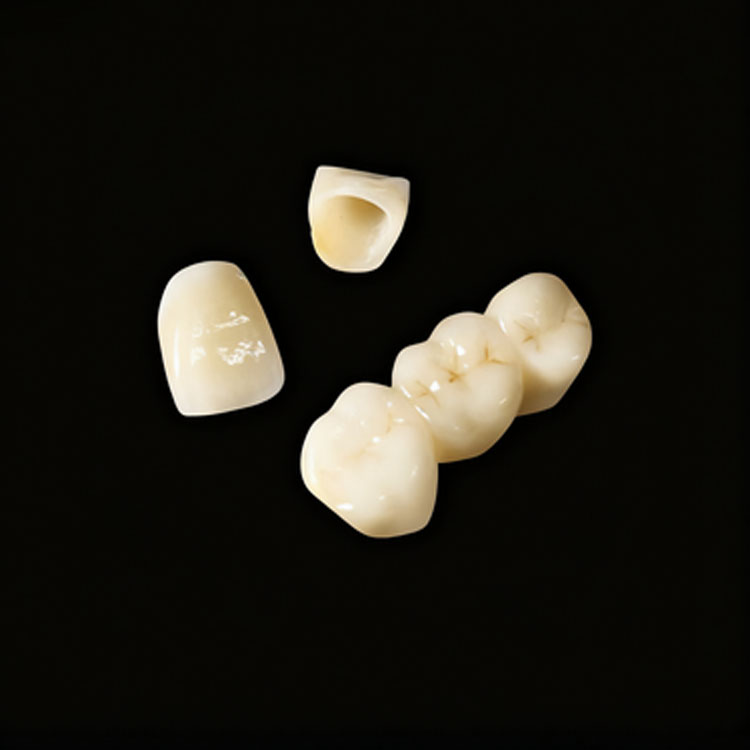
Вот мое прямое мнение.
Если зуб все еще остается в основном эмалевым, то винир E.max обычно является более разумным решением. Если зуб стал структурным, то коронка E.max обычно является более честным решением.
Звучит просто, но это противоречит тому, как часто продают этот рынок. Обзор виниров Кливлендской клиники Виниры по-прежнему используются в качестве косметической оболочки для устранения сколов, щелей, обесцвечивания и проблем с формой, в то время как руководство по коронкам Американского колледжа ортопедов коронки ставят на сломанные зубы, очень большие пломбы, зубы с корневым каналом и изношенные зубы от стачивания. Это граница на простом английском языке: винир - когда вы в основном меняете внешнюю сторону, коронка - когда вы пытаетесь спасти весь видимый зуб.
И да, материал вносит разнообразие в разговор. IPS e.max - это дисиликат лития, Li₂Si₂O₅, и Ivoclar продает его в широком диапазоне показаний: IPS e.max CAD при прочности на изгиб 530 МПа, и IPS e.max Press для всего: от тонких виниров 0,3 мм до передних и боковых коронок. Одно и то же семейство керамики. Разные биологические цены.
Я проверил структуру сайта.
Иерархия не является тонкой.
Сайт стандартный процесс работы с винирами E.max позиционируется как сбалансированный вариант дисиликата лития для консервативных косметических случаев с одним или несколькими блоками. полный вариант виниров E.max В основе лежит предсказуемая посадка, контроль за оттенком и согласованность нескольких частей. Многослойное наращивание виниров E.max зарезервирован для премиальной передней характеристики, а Страница с коронками E.max для передних реставраций опирается на полупрозрачность, анатомию и прочность. Это не случайная навигация. Это карта материального риска, спрятанная у всех на виду.
Мне особенно нравится одна внутренняя ссылка: сайт руководство по координации материалов для полного рта открыто разделяет полные виниры E.max, многослойные виниры E.max, коронки E.max, многослойные коронки из диоксида циркония и полноконтурные многослойные циркониевые коронки по зонам и степени риска. Это умнее, чем обычная рекламная копия, потому что признает суровую истину: красота передних зубов и выживание задних - не одно и то же задание.
Вот тут-то и начинается настоящий спор.
Не бренд. Биологическая реальность.
Систематический обзор и мета-анализ 2024 года в Журнал ортопедической стоматологии обнаружили, что керамические виниры, приклеенные к эмали или с минимальным воздействием на дентин, показали очень хорошие результаты, но сильное воздействие на дентин привело к снижению выживаемости до 91% и успеха до 74%. Это не ошибка округления. Это вся история выбора случая. Меня не волнует, насколько красиво выглядит макет, если препарирование уже прожгло слишком много эмали.
Затем в ретроспективном исследовании 2025 года за 672 керамическими винирами 189 пациентов наблюдали в течение 1-15 лет и снова обнаружили, что степень обнажения дентина значительно влияет на выживаемость. Суть та же, набор данных другой: как только вы покидаете страну эмали, предсказуемость виниров начинает вести переговоры с физикой. Хотите более чистый способ сказать это? Если вы проводите бондинг на дентине, потому что препарирование, предыдущие реставрации или износ вынудили вас к этому, вы уже приблизились к границе показаний.
Именно поэтому я бы, естественно, обратил внимание читателей, сравнивающих эстетические возможности, на сайт стандартная страница виниров E.max и полная страница виниров E.maxИ то, и другое явно построено на консервативной логике виниров, а не на героической спасательной стоматологии.
Теперь о самом непопулярном.
Коронки не являются автоматическим избыточным лечением. Иногда это первый правдивый план лечения на столе.
Если зуб расколот, сильно восстановлен, подвергся эндодонтическому лечению, сильно изношен или в нем отсутствует слишком большая окружная структура, покрытие коронками - это не косметический театр. Это управление нагрузкой. На сайте Американская ассоциация эндодонтистов утверждает, что при лечении трещин на зубах следует устанавливать коронки, ссылаясь на данные о том, что ранняя установка коронок может улучшить прогноз на 98% за 11 лет; другой источник AAE сообщает о 94% двухлетней выживаемости для эндодонтически вылеченных трещин на зубах, на которые были установлены коронки, против всего 20% без коронок. Такие цифры быстро заканчивают дискуссии в Instagram.
Да и сами характеристики коронок не являются тем слабым звеном, за которое их выдают критики. В обзоре доказательной базы 2025 года, охватывающем около 35 000 коронок, сообщается, что коронки из дисиликата лития обеспечивают от 95% до 100% краткосрочной и среднесрочной выживаемости, при этом износ эмали антагонистов описан как минимальный, если поверхности правильно отполированы. Так что да, биологическая стоимость коронки выше. Но механическая выгода может быть полностью рациональной, когда зуб больше не является структурно надежным.
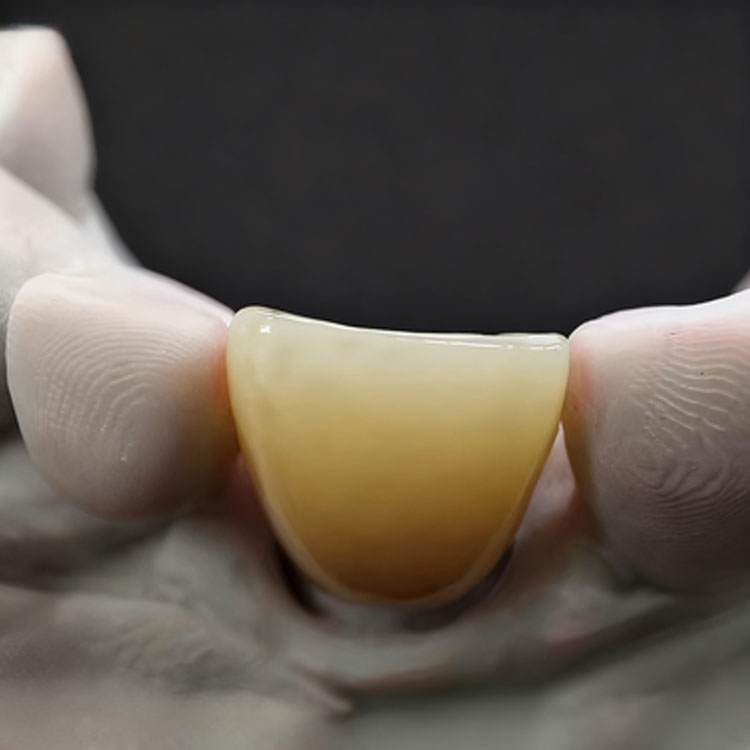
Я все делаю просто.
Потому что репейнику нет дела до маркетинговых формулировок.
| Клиническая переменная | E.max винир | E.max корона | Моя жесткая правда |
|---|---|---|---|
| Оставшаяся эмаль лица | Почти не поврежден | Часто уменьшается или становится пятнистым | Если вы все еще владеете эмалью, защитите ее |
| Экспозиция дентина после препарирования | Минимум | Умеренная или обширная приемлемая | Как только дентин становится основным материалом, риск установки виниров возрастает |
| Существующие реставрации | Небольшой или умеренный | Крупные MOD, множество старых композитов, большое наращивание | Старая стоматология обычно выдвигает коронку вперед |
| Состояние трещин | Нет структурных трещин | Трещина, компромисс зубцов, синдром трещины | Треснувший зуб - это не случай тщеславия |
| Эндодонтический статус | Предпочтительно наличие витального зуба | Часто встречается после РКТ или глубокой структурной потери | Логика коронки становится более прочной после эндодонтии |
| Износ / бруксизм | Легкий, управляемый | Умеренная и тяжелая нагрузка | Парафункция наказывает за красивые идеи |
| Основная цель | Цвет, форма, незначительное положение, утонченность улыбки | Армирование плюс эстетика | Винир меняет лицо; коронка спасает оболочку |
| Неудача, которой вы боитесь больше всего | Дебонд, край излома, несоответствие цвета | Завышенные затраты на подготовку, нехватка маржи, сколы/изломы | Выбирайте тот вариант отказа, с которым вы можете смириться |
Эта таблица не является теорией. Это совпадение данных по выживаемости виниров, литературы по трещинам зубов, обзоров выживаемости коронок и того, как сама лаборатория Artist Dental Lab разделяет Виниры E.max, полные виниры E.max, Многослойные виниры E.max, и Коронки E.max.
Я скажу прямо.
Самая большая ошибка - использовать язык виниров в случаях с коронками, потому что “минимально инвазивный” продается лучше.
Зуб с широким обнажением дентина, глубокой линией трещины, огромным старым композитом или историей корневого канала не подходит для винира, потому что дисиликат лития красив. Он становится неудачей винира, которая только и ждет, чтобы случиться. С другой стороны, я также считаю, что некоторые врачи слишком быстро готовят коронки, когда дисциплинированный винир на основе эмали справился бы с задачей с меньшим биологическим ущербом. Обе ошибки происходят от одной и той же вредной привычки: рассматривать реставрацию как звезду, а субстрат - как побочный элемент. Эта привычка стоит дорого.
Есть также угол зрения на рабочий процесс, который большинство людей упускают. Чем больше дело зависит от контроля оттенков, точности редукции, качества фотографий, управления стоимостью и гармонии между единицами, тем больше вам нужна лаборатория, которая действительно разделяет “сбалансированный повседневный E.max”, “полную последовательность E.max” и “многослойный артистизм E.max” вместо того, чтобы сваливать все три под один красивый ярлык. Artist Dental Lab разделяет их, и, честно говоря, это правильный шаг.
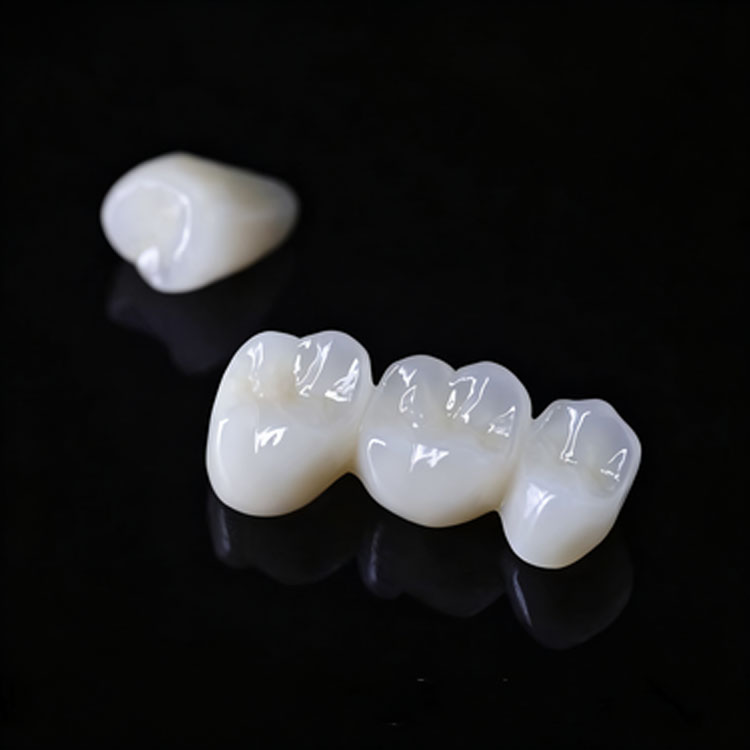
Виниры E.max - это тонкие реставрации на литий-дисиликатной основе, используемые в основном в тех случаях, когда зуб остается структурно здоровым и сохраняет достаточно эмали для надежной адгезии, а коронки E.max - это реставрации с полным покрытием, используемые, когда зуб нуждается в окружном укреплении из-за перелома, лечения корневого канала, сильного износа или больших реставраций, изменивших профиль риска. Тогда настоящая работа заключается в подборе биологии к покрытию, а не в погоне за более мягкими условиями продаж.
Лучший способ выбрать между винирами и коронками E.max для поврежденных передних зубов - это оценить, насколько неповрежденными остались эмаль, дентин, расширение трещины и окружная структура зуба, потому что виниры лучше всего работают в косметических случаях с преобладанием эмали, а коронки - когда зуб уже нуждается не только в эстетическом улучшении, но и в структурной защите. Я бы не позволил “переднему зубу” обмануть вас, чтобы не лечить структурную проблему.
Виниры E.max часто лучше для консервативной эстетики, когда положение зуба, объем эмали и условия бондинга благоприятны, а коронки E.max лучше, когда эстетика должна сосуществовать с серьезным структурным компромиссом, потому что красивая коронка на поврежденном зубе почти всегда выигрывает у хрупкого винира на том же зубе. Я знаю, что это звучит жестко, но переделки еще жестче.
Обнажение дентина начинает подталкивать винир к коронке, когда препарирование теряет преимущество бондинга на основе эмали, особенно если обнажение дентина обширно, поскольку данные систематического обзора показывают значительно худшую выживаемость и успех, когда обнаженный дентин становится основной частью субстрата для бондинга. Именно эту линию пропускают многие глянцевые презентации случаев.
Коронки из дисиликата лития достаточно долговечны с клинической точки зрения для многих передних и некоторых задних зубов с одной коронкой. В последних обзорах доказательной базы сообщается о краткосрочной и среднесрочной выживаемости в диапазоне 95% - 100% и минимальном износе эмали антагонистов, если поверхность правильно отполирована и случай хорошо подобран. Достаточная прочность - не то же самое, что универсальность, но она гораздо лучше, чем предполагают критики.
Мой совет прямолинеен.
Определите субстрат, прежде чем приступать к реставрации.
Если вы пишете для стоматологов, покажите читателям реальный контрольный список: остаток эмали, процент обнажения дентина, объем существующей реставрации, состояние трещин, жизнеспособность, окклюзионная нагрузка, оттенок культи, а также то, является ли случай восстановлением улыбки или спасением конструкции. Если вы строите клинический или лабораторный рабочий процесс на основе этой логики, я бы начал с сайта Путь из шпона E.max для сбалансированных консервативных случаев полный путь виниров E.max для контролируемой многокомпонентной последовательности. многослойная дорожка из шпона E.max для определения истинной передней части премиум-класса, и Путь к коронкам E.max или даже многослойное циркониевое покрытие на весь контур когда случай уже перешел от косметической доработки к управлению структурой. И если вы хотите, чтобы лаборатория была задействована как можно раньше, отправьте сканы, тени культи, записи о редукции и фотографии до того, как история подготовки будет переписана оптимизмом в кресле.