


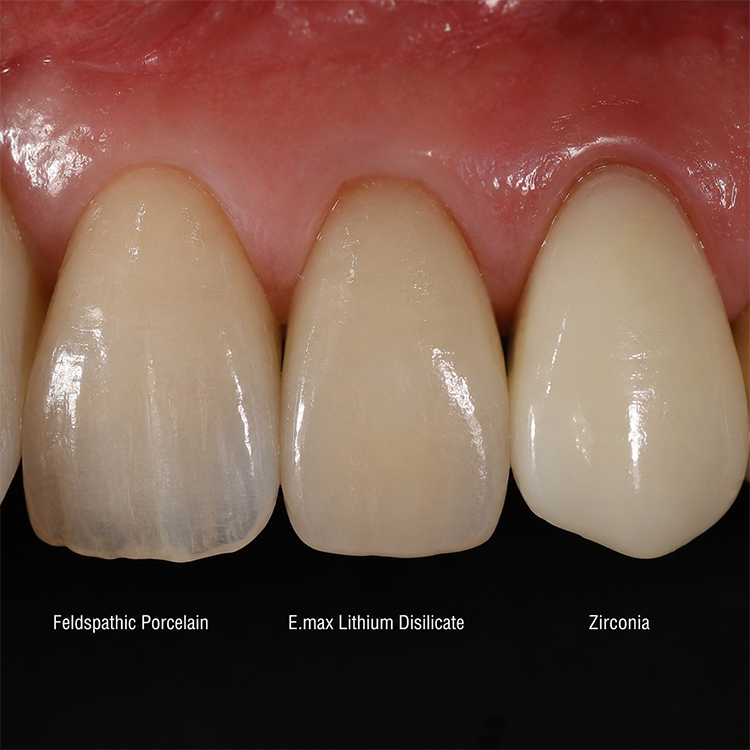
Margin structure decides whether ceramic restorations seat cleanly, look alive, and survive function. Here is the hard comparison most material brochures avoid.
Margins expose everything.
A crown or veneer can photograph beautifully on a lab bench, with incisal glow, polished anatomy, and a shade tab sitting nearby like a marketing prop, but if the dental crown margin design is vague, over-thinned, unsupported, or mismatched to the ceramic, the restoration becomes a delayed argument between biology, cement, ceramic thickness, and chairside patience.
So why do we still talk about Feldspathic vs E.max vs Zirconia like this is mainly a “beauty versus strength” debate?
I have a hard opinion here: the material is not the hero. The margin is. The material only tells you how much punishment the edge can tolerate before the case starts demanding excuses.
Feldspathic porcelain, E.max lithium disilicate, and zirconia are not three flavors of “premium ceramic.” They are three different risk contracts. Feldspathic porcelain buys you enamel-like light behavior and punishes bad support. E.max, built around lithium disilicate glass-ceramic chemistry often discussed as Li₂Si₂O₅, gives you more structure and broader indication discipline. Zirconia, ZrO₂, especially modern multilayer systems using 3Y-TZP and 5Y-PSZ zones, gives you higher strength and thinner-wall options, but it still needs a finish line a scanner, mill, technician, and clinician can actually read.
That is why I would never separate material choice from preparation geometry. Artist Dental Lab’s own zirconia crowns vs E.max crown margin guide makes the same point from the lab side: margin design is not a small technical footnote; it is where remake risk begins.
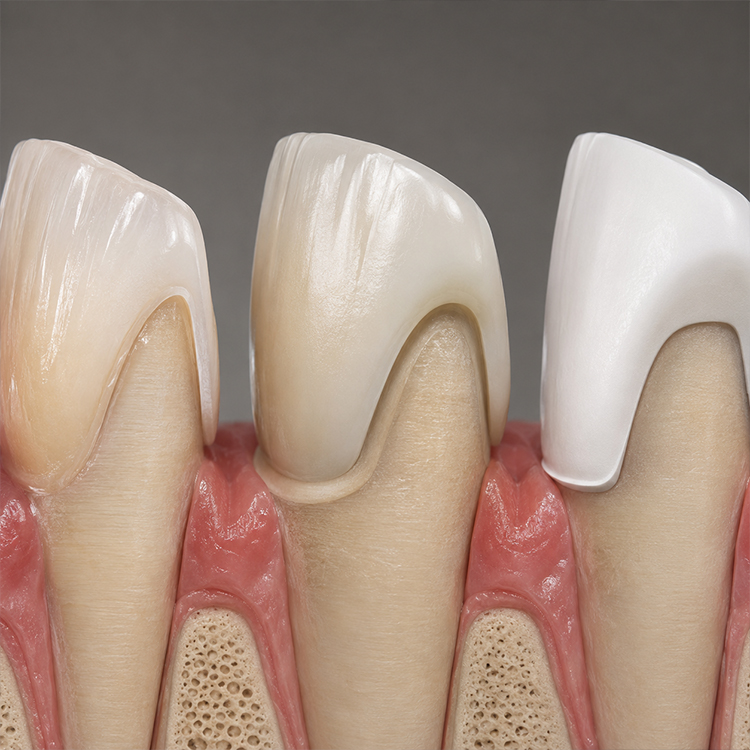
Feldspathic is seductive.
It is also the material most likely to embarrass a sloppy plan, because the same thinness and translucency that make a feldspathic veneer look alive also make it less forgiving when the tooth is dark, the margin is unclear, the reduction is uneven, or the clinician expects a hand-layered ceramic shell to perform like a structural crown.
The best use case is narrow and real: anterior veneers, enamel-preserving preparations, controlled shade change, delicate incisal effects, and a patient whose esthetic demand justifies the labor. Artist Dental Lab’s Pagina di impiallacciatura feldspatica correctly frames it around hand-layered translucency, micro-texture, conservative preparation, and clear margin notes. That is the right language. Not “strong.” Not “universal.” Not “works everywhere.”
The evidence is more favorable than some zirconia loyalists admit. A retrospective clinical study of 170 feldspathic ceramic veneers reported a 91.77% survival rate for up to 7 years, with failures at 8.23%, according to the 2022 PMC-indexed study on feldspathic ceramic laminate veneers. A later systematic review and meta-analysis reported a pooled survival rate of 96.13% for feldspathic veneers at a mean 10.4 years, as summarized in this 2024 PMC systematic review of ceramic veneer survival.
But those numbers should not be abused.
They do not mean feldspathic porcelain is mechanically forgiving. They mean feldspathic can last when the case is selected well, bonded well, finished well, and maintained well. Different statement. Very different bill.
For feldspathic veneer margin design, I want the margin placed where the ceramist can preserve thin optical transition without creating a bulky cervical ledge. Window, butt-joint, and incisal-wrap designs can all work, but the decision should follow enamel volume, occlusion, tooth shade, smile line, and required length change. If the patient wants bleach-shade masking over a dark stump with almost no reduction, feldspathic is not “premium.” It is a trap wearing lipstick.
E.max gets oversold.
The market talks about E.max like it solved the ceramic compromise forever, but lithium disilicate still has rules, and when people ignore those rules, they usually blame the lab, the scanner, the mill, the cement, or the patient’s bite before admitting the prep never gave the material a fair margin.
Ivoclar’s own technical literature is more honest than many sales pages. The IPS e.max CAD/Press adhesive 1 mm crown guide states that IPS e.max lithium disilicate, at 500 MPa in that document and with IPS e.max CAD reported at 530 MPa mean biaxial flexural strength, permits a crown layer thickness of at least 1.0 mm only when used with adhesive cementation, and it calls for a circular shoulder or chamfer at least 1.0 mm wide, with rounded internal edges, according to the official Ivoclar adhesive 1 mm crown guide.
That sentence matters.
It means “1 mm E.max” is not a slogan. It is a conditional protocol. Adhesive cementation. Anatomical support. No sharp edges. No bruxism in that specific indication list. No pretend-retentive prep that asks a glass-ceramic margin to survive on optimism.
For E.max crown preparation margins, I like a rounded shoulder or a well-formed deep chamfer. I dislike knife-edge thinking unless a very specific indication and material protocol supports it, and even then I want documentation. Lithium disilicate can be beautifully predictable in anterior crowns and select posterior cases, but the margin must protect ceramic thickness and avoid cervical overcontour.
That is where the E.max crowns workflow deserves an internal link in this article. The page asks for STL scans, margin notes, shade, stump shade, photos, and occlusal guidance. Good. That is not paperwork. That is margin insurance.
For veneers, the E.max veneer page makes another useful distinction: lithium disilicate veneers are not just about translucency; they are about predictable fit, strength, and communication of margin and reduction notes. I would use E.max over feldspathic when I need a stronger ceramic architecture, more moderate shade management, or better repeatability across multiple units.
But I would still not call it forgiving. E.max remembers bad geometry. It just complains later.
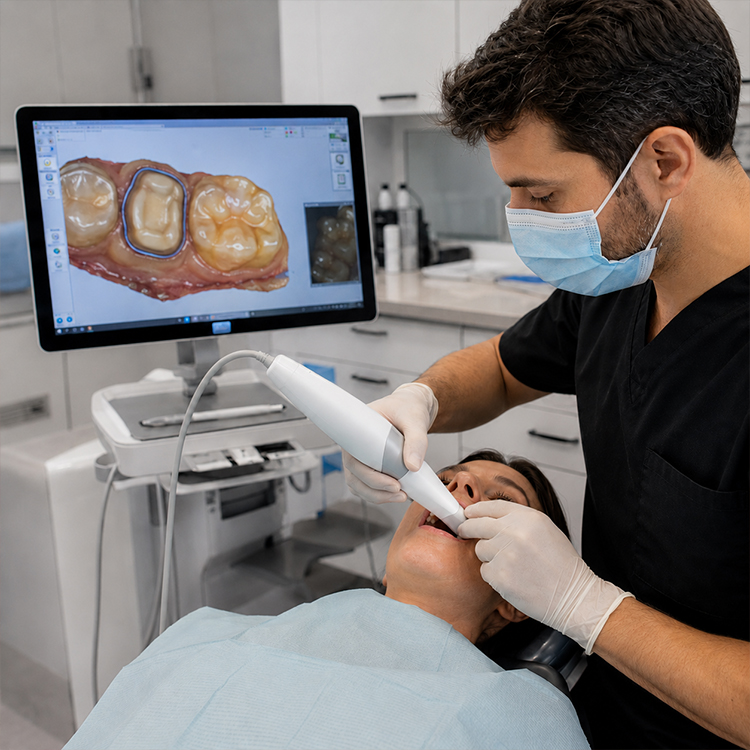
Zirconia forgives more.
That does not mean zirconia forgives everything, and this is where I think a lot of clinicians, milling centers, and low-price labs get reckless. High flexural strength does not rescue unreadable margins, sharp internal line angles, poor seating space, wet bonding theater, or an emergence profile that looks like it was designed by a spreadsheet.
Modern zirconia is not one thing. A multilayer zirconia block may use strong 3Y-TZP in the dentin body and more translucent 5Y-PSZ toward the incisal zone. Ivoclar’s IPS e.max ZirCAD Prime block page reports 1,100 MPa flexural strength and says that strength allows crown wall thickness down to 0.8 mm; it also describes the material transition from 3Y-TZP zirconia to 5Y-PSZ zirconia for translucency, according to Ivoclar’s ZirCAD Prime technical product page.
So yes, zirconia can run leaner than E.max in many crown situations. But no, zirconia crown finish line design is not optional.
A 2020 systematic review on tooth-supported zirconia single crowns found that shoulder finish-line preparations had slightly better marginal fit than chamfer finish lines, according to this PMC-indexed systematic review on zirconia crown fit. I do not read that as “never use chamfer.” I read it as: stop pretending finish-line geometry has no measurable effect.
For posterior strength cases, bridge workflows, implant-supported restorations as prescribed, and bruxism-adjacent risk profiles, zirconia often wins the conversation early. Artist Dental Lab’s pagina in zirconia multistrato full-contour frames the material around CAD/CAM precision, monolithic anatomy, reduced porcelain chipping risk, and posterior function. That is the right lane.
The danger starts when zirconia is chosen because nobody wants to confront the prep. If the finish line is messy, subgingival beyond visibility, or digitally stitched into fiction, zirconia may still mill. It may still seat. It may even pass the mirror test. But the tissue usually knows.
This is the practical split I would use when reviewing margin structure across Feldspathic vs E.max vs Zirconia.
| Factor | Feldspathic Porcelain | E.max / Lithium Disilicate | Zirconia |
|---|---|---|---|
| Core chemistry | Feldspathic porcelain glass matrix | Lithium disilicate glass-ceramic, often described as Li₂Si₂O₅ | Zirconium dioxide, ZrO₂; may include 3Y-TZP and 5Y-PSZ zones |
| Typical strength logic | Esthetic shell; depends heavily on bonding and support | Middle-strength structural ceramic; IPS e.max CAD commonly cited around 530 MPa | High-strength ceramic; ZirCAD Prime cited at 1,100 MPa |
| Margin personality | Needs enamel support and delicate transition | Needs rounded support and thickness discipline | Tolerates thinner walls better, but still needs readable geometry |
| Common finish-line preference | Veneer-specific window, butt-joint, or incisal wrap depending on case | Rounded shoulder or deep chamfer; commonly around 1.0 mm for crowns under certain protocols | Shoulder or chamfer; often can support reduced wall thickness depending on system |
| Best esthetic lane | Thin anterior veneers, subtle characterization, enamel-like translucency | Anterior crowns, veneers, moderate masking, repeatable esthetics | Posterior crowns, bridges, high-force cases, monolithic workflows |
| Rischio di guasto principale | Fracture, debonding, overcontour, poor masking | Thin cervical ceramic, adhesive errors, unsupported margins | Poor fit from unreadable prep, low-translucency compromises, cementation protocol errors |
| My blunt call | Best when the tooth is already kind | Best when beauty and structure both matter | Best when function gets ugly |
The remake is rarely mysterious.
When a case comes back, everyone starts defending their corner. The clinician says the scan was good. The lab says the margin was unclear. The patient says the crown feels bulky. The sales rep says the material is strong. Somewhere inside that mess sits the truth: the ceramic was asked to solve a geometry problem.
A 2023 in-vitro comparison of contemporary dental ceramics found that lithium disilicate crowns had clinically acceptable marginal accuracy and that zirconia and zirconia-reinforced lithium silicate materials could produce favorable results under controlled conditions, according to the PMC study on marginal discrepancy of five contemporary dental ceramics. That is useful, but it should humble us. Lab conditions are not saliva, blood, tissue collapse, soft scans, time pressure, and a patient asking whether the crown can be seated before lunch.
Clean margins sell predictability. Bad margins sell drama.
The commercial lesson is uncomfortable: a dental lab that accepts every material request without challenging preparation, clearance, shade masking, and margin design is not being service-minded. It is being lazy. And a clinic that sends vague scans and expects “premium ceramic” to cover the lack of planning is not saving time. It is outsourcing risk.
That is why I like using Artist Dental Lab’s case-based guide to E.max, zirconia, and feldspathic anterior veneers as a decision checkpoint before material selection becomes emotional. The better question is not “Which ceramic is best?” The better question is: what margin structure can this tooth honestly support?
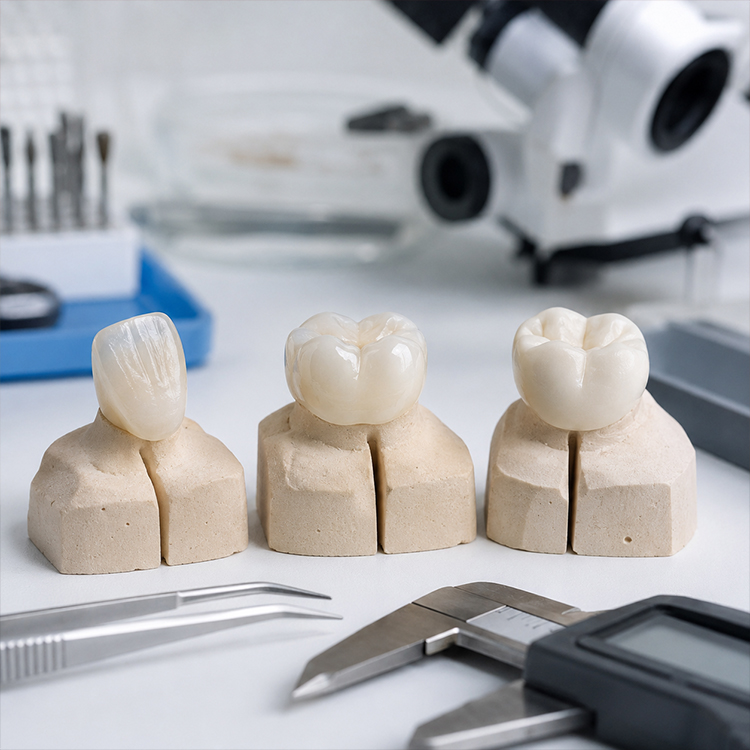
I would lean feldspathic when the preparation stays mostly in enamel, the patient needs delicate anterior characterization, the target shade is not wildly brighter than the underlying tooth, and the clinician can provide photos, stump shade, smile-line context, and a margin the ceramist can finish without guessing.
Thin wins here.
But thin only wins when the case is kind. If the prep is into dentin everywhere, the tooth is dark, the patient bruxes, the incisal edge is functionally hostile, or the margin disappears into a scan shadow, feldspathic stops being elegant and starts being fragile.
I would lean E.max when the case needs more structure than feldspathic but still demands high esthetics: anterior crowns, premolar veneers, moderate color correction, and multi-unit smile work where repeatability matters more than one heroic incisal effect.
The E.max margin should be defined, rounded, and thick enough to avoid a weak cervical edge. If the clinician wants a 1.0 mm crown, I want the conversation to include adhesive cementation, occlusion, anatomical support, and the manufacturer’s restrictions. Otherwise, “minimal prep” becomes a legal-looking phrase for under-reduction.
I would lean zirconia when load dominates: posterior crowns, bridge cases, limited clearance, implant-supported restorations as prescribed, bruxism risk, or patients who have already taught the team that porcelain layering is a gamble.
Still, I want a clean margin. Zirconia is strong, not psychic. If the scan cannot read the finish line, the mill cannot respect it, and the technician cannot design confidently around it. That is not material science. That is wishful billing.
Dental crown margin design is the planned finish-line geometry where the prepared tooth meets the restoration, controlling ceramic thickness, seating accuracy, cement behavior, emergence profile, tissue response, and long-term fracture risk across materials such as feldspathic porcelain, E.max lithium disilicate, and zirconia. It is the structural boundary of the case.
In practice, this means the clinician must choose a margin that the tooth, material, scanner, mill, ceramist, and cementation protocol can all tolerate. A beautiful crown with a bad margin is not a success. It is a delayed remake.
The best margin design for ceramic crowns is usually a smooth rounded shoulder or well-formed chamfer that provides enough ceramic bulk, avoids sharp internal corners, supports accurate scanning or impression capture, and matches the selected material’s strength, translucency, and cementation protocol. The right answer changes by ceramic type.
For E.max crowns, I usually want disciplined thickness and a rounded support form. For zirconia, I may accept a leaner design when the system allows it, but I still want a readable finish line. For feldspathic veneers, I care more about enamel support and optical transition than crown-style reduction.
E.max crown preparation margins generally require more respectful ceramic thickness and adhesive planning, while zirconia margins can often tolerate thinner wall dimensions because modern zirconia systems have much higher flexural-strength values and different cementation options. The tradeoff is that zirconia still needs clean, visible, millable geometry.
The mistake is treating zirconia strength as a substitute for preparation quality. E.max punishes thin unsupported margins faster, but zirconia can still fail esthetically, biologically, or fit-wise if the finish line is vague or the emergence profile is overbuilt.
Feldspathic veneer margin design is usually more dependent on enamel preservation, thin optical transition, and delicate hand-layered contour, while E.max veneer margin design can tolerate broader structural use because lithium disilicate provides higher strength and more repeatable CAD/CAM or pressed workflows. Both still demand clean margins.
I would not use feldspathic just because it sounds premium. I would use it when the tooth allows conservative preparation and the esthetic goal needs that enamel-like light behavior. E.max is often the safer compromise when the case needs more structure.
Choose crown margin design by matching the finish line to the ceramic’s mechanical limits, optical goals, cementation protocol, tooth shade, remaining enamel, occlusion, scanner readability, and required wall thickness, rather than choosing the material first and forcing the preparation to obey later. Margin logic should lead material selection.
My shorthand is simple: feldspathic for thin enamel-driven anterior beauty, E.max for esthetic structure with margin discipline, and zirconia for higher-load situations where strength and reduced chipping risk matter more than maximum translucency.
Do not start your next ceramic case by asking, “Feldspathic, E.max, or zirconia?”
Start with the margin.
Send the lab clear STL scans, prep photos, stump shade, reduction notes, occlusal guidance, smile photos, and a brutally honest statement of what the restoration must hide, survive, or imitate. If the margin cannot support the material, change the prep, change the material, or change the promise.
For B2B cases where dental crown margin design is driving the risk, contact Artist Dental Lab and start with a trial case that includes margin notes, shade documentation, and material goals before production begins. That is how serious teams reduce remakes. That is how the ceramic gets a fair chance.