


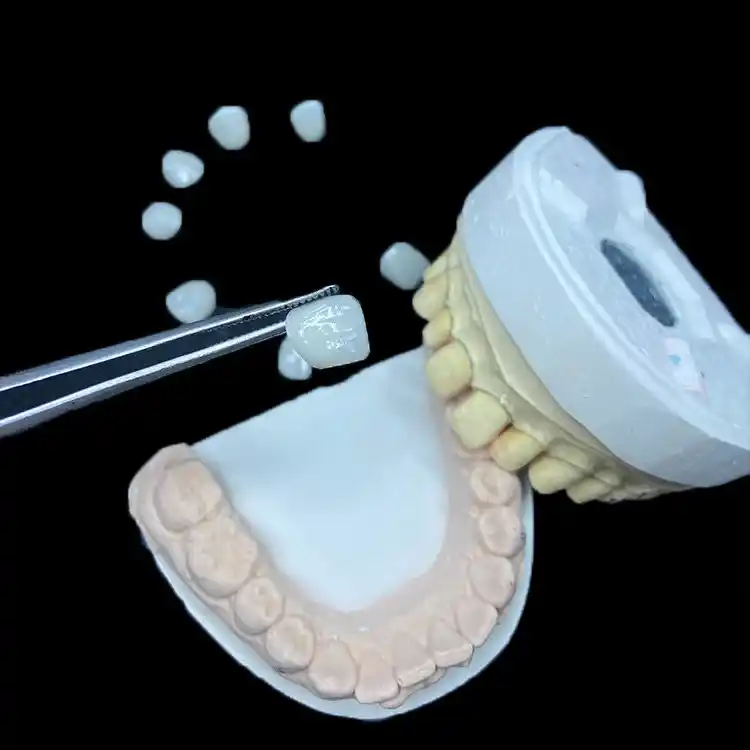
I confront the “Veneer Selection” dilemma with frank industry insight, backed by clinical comparisons of E.max vs feldspathic veneers, performance data, and laboratory links you can actually use.
Not magic. Just ceramics.
But if you’ve ever watched a ceramist chase an incisal halo while the prep is “kinda sorta” in enamel, the stump shade is missing, and the doc wants zero opacity with zero reduction, you already know the real question isn’t “E.max vs feldspathic”—it’s “what failure mode am I willing to babysit?”
And yeah… are we being honest about the occlusion?
If you’ve ever watched a ceramist stack porcelain at 11 p.m. while the dentist texts “one more tweak,” and the patient demands TikTok-white value on a thin, dehydrated shade tab, you already know veneer selection is an argument about physics, not vibes.
It cracks. Fast.
So I’m going to be blunt: I frankly believe a lot of “esthetic veneer planning” is just people hiding from the boring stuff—functional scheme, parafunction, bonding discipline, and whether the case is even eligible for ultra-thin porcelain without turning into a remake factory.
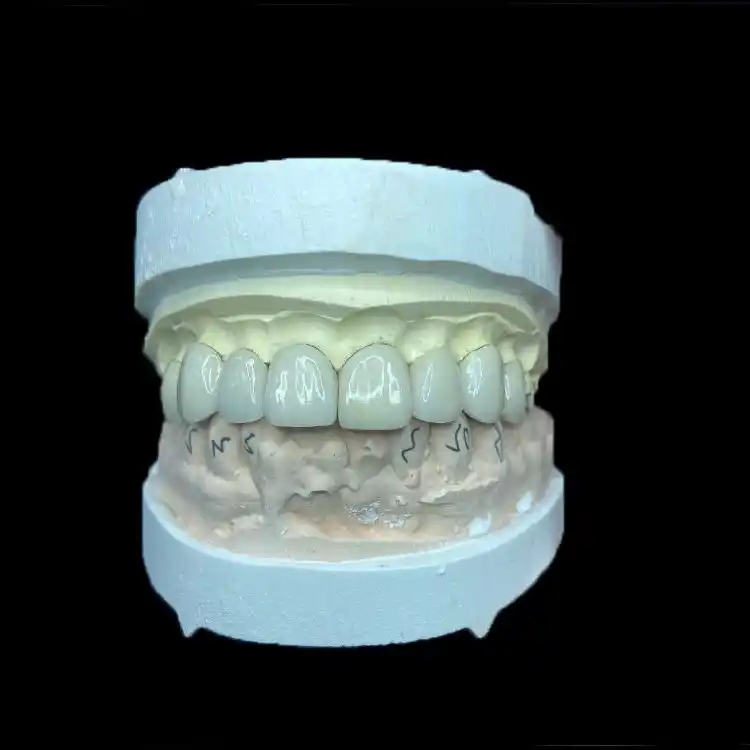
E.max is lithium disilicate (think Li₂Si₂O₅), the workhorse glass-ceramic that can take a beating compared to classic porcelain, and it’s why so many labs push it for predictable outcomes. The flexural strength numbers people throw around are usually in that ~360–400 MPa neighborhood.
Feldspathic is the old-school, hand-layered stuff—microtexture, light dynamics, that “enamel-y” sparkle when the patient turns their head under mixed lighting. It’s gorgeous. It’s also less forgiving when the bite is spicy or the prep forces thickness compromises. Artist Dental Lab literally frames it as “hand-layered feldspathic veneers” aimed at premium anterior esthetics, minimal-prep cosmetic cases, and delicate incisal characterization—translation: it wants a controlled environment.
And here’s the ugly truth: when a veneer fails, it usually isn’t “because the material is bad.” It’s because somebody ignored the margin design, reduction notes, stump shade, or bonding protocol (or—my favorite—pretended a bruxer “doesn’t grind”).
Let’s talk data, not dentist folklore.
A 2024 meta-analysis in Journal of Esthetic and Restorative Dentistry reported pooled survival rates around 96.13% for feldspathic and 96.81% for lithium disilicate over roughly a decade-ish observation window (yes, survival is close; complications are where the story gets messy).
Now the part that actually changes how I treatment-plan: a university-hosted clinical evaluation following 197 CAD/CAM laminate veneers (feldspathic VMII vs lithium disilicate EmaxCAD) tracked up to 10 years and found Kaplan–Meier survival about 92.7% for EmaxCAD vs 89.1% for VMII, with location mattering (incisors behaving better than canines/premolars). That’s not marketing—that’s the “your canine guidance can ruin your day” footnote made real.
And if you think the veneer boom is all high-end dentists doing perfect dentistry… nah. In May 2024, the ADA publicly warned about unlicensed “veneer techs,” and AP News covered arrests tied to social-media veneer scams—patients lured by low prices, then left with irreversible damage. That’s the shadow market sitting right next to the legit one.
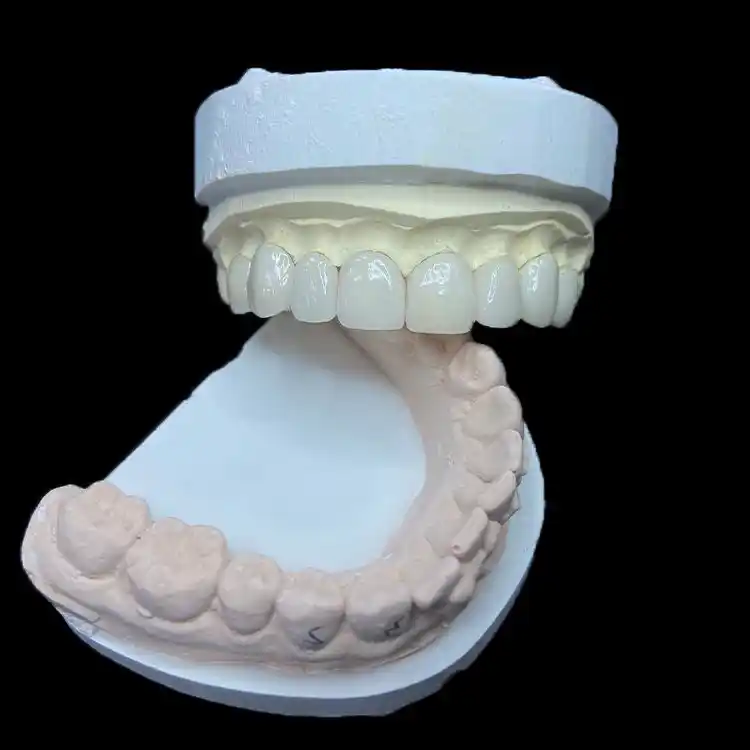
Yet the lab is where the lies show up.
One day you get an “E.max veneer case” with margins that disappear into saliva-contaminated scans, no stump shade, and a note that says: “BL1, natural.” The next day it’s feldspathic requested at 0.2–0.3 mm everywhere (cute) on a patient who clenches like it’s their job. Then the doc is shocked when you recommend a different material or a different design (wrap vs window vs butt-joint).
If you want to see how a lab frames indications in plain English, Artist Dental Lab is unusually direct about “best for,” “prep guidance,” and what to send—photos, stump shade, reduction notes, occlusion guidance—aka the stuff that decides whether the veneer looks like enamel or looks like a bathroom tile. Start with their product hub.
And if you’re comparing lab philosophies, it’s useful to peek at other all-ceramic menus too.
Three rules I use (and yes, I break them sometimes, then regret it):
If you want internal, product-specific references (not vague blog fluff), here are the pages I’d actually hand to a colleague:
| Criterion | E.max Veneer | Feldspathic Veneer |
|---|---|---|
| Flexural Strength | 360–400 MPa (lithium disilicate) | ~60–120 MPa (porcelain) (pmc.ncbi.nlm.nih.gov) |
| Translucency | Slightly opaque, still high | Superior translucency |
| Ideal Indication | Bruxers, functional loads | Minimal prep esthetic zones |
| Preparation | Moderate enamel reduction | Ultra-thin or minimal |
| Long-Term Complications | Lower | Slightly higher |
| Predictability | High (CAD/CAM) | Depends on ceramist skill |

What are the key differences between E.max and feldspathic veneers?
E.max veneers are lithium disilicate ceramic shells built for higher fracture resistance and more consistent thickness control, while feldspathic veneers are hand-layered porcelain laminates optimized for enamel-like translucency, microtexture, and incisal characterization—usually with a lower tolerance for occlusal abuse and protocol sloppiness.
In real life, it’s strength-and-repeatability versus artistry-and-optics. Pick your tradeoff.
How do I choose between E.max vs Feldspathic based on occlusal forces?
Occlusal-force selection is the process of matching veneer material and design to functional load (bruxism, guidance patterns, contact points) so failure risk shifts from catastrophic fracture to manageable wear or minor chipping, ideally while preserving enamel bonding and thickness targets for shade control.
If the patient clenches, I lean E.max and stop pretending minimal-prep porcelain is “safe.”
Can feldspathic veneers be as long-lasting as E.max?
Longevity equivalence means feldspathic and lithium disilicate veneers can show similar long-term survival percentages in well-selected cases, but the day-to-day reality is complication profiles differ—debonding, chipping, and fracture patterns show up depending on tooth position, thickness, and bonding/occlusion execution.
That 2024 meta-analysis survival closeness is real; the “how” behind it is where clinicians get burned.
What’s the biggest hidden driver of veneer failure?
The biggest hidden driver is not the ceramic brand—it’s workflow discipline: margin clarity, reduction mapping, stump shade/value targets, contamination control, and adhesive protocol consistency, because veneers are thin shells that magnify every small mistake into shade mismatch, marginal leakage, or debonding over time.
I’ve seen “perfect” ceramics fail from lazy records.
Why are “veneer tech” stories relevant to material selection?
The “veneer tech” issue matters because it shows how veneers are treated as a commodity procedure rather than irreversible restorative dentistry, and that mindset bleeds into legitimate settings—rushed preps, skipped diagnostics, bargain bonding, and patients trained to demand looks over biology.
In 2024, both AP News and the ADA publicly warned about this trend for a reason.
Want fewer remakes and fewer “why does it look gray?” chairside surprises? Send better records, pick the material that matches the occlusion you actually have (not the one you wish you had), and lean on a lab that states indications clearly—start with the Artist Dental Lab product pages above and run a trial case through their workflow.