


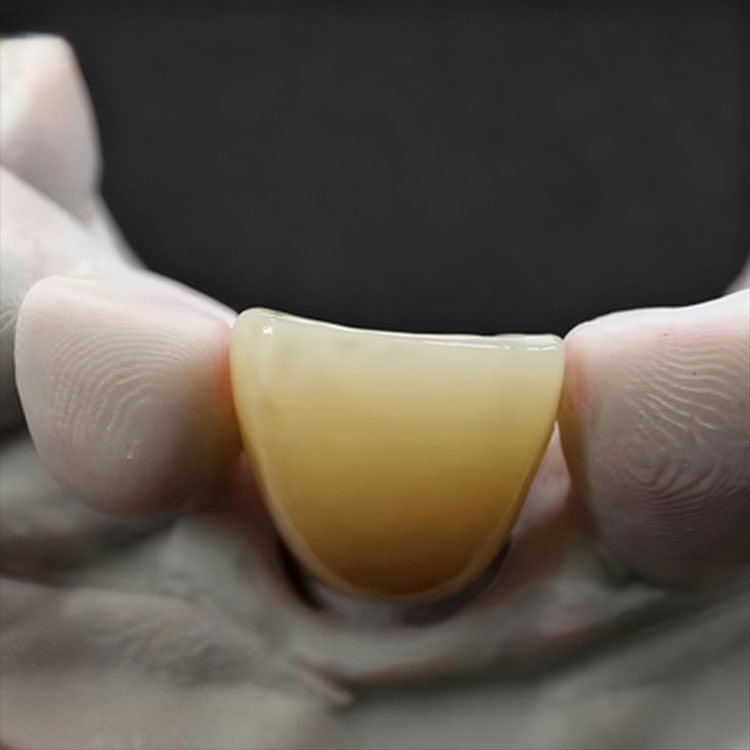
Feldspathic is not dead. E.max is not magic. The better veneer material depends on enamel, stump shade, prep space, occlusion, unit count, and whether the case needs artistic invisibility or mechanical control.
Feldspathic is not the nostalgic museum piece some digital labs pretend it is. E.max is not the miracle ceramic some chairside sales decks make it sound like. In the real feldspathic vs Emax veneers debate, the winner is usually decided before the case ever reaches the furnace: enamel volume, stump shade, prep discipline, incisal effect demand, parafunction risk, cement shade, and how honest the dentist was with the lab.
That part matters.
I have seen smile makeover cases where lithium disilicate was the safer, cleaner, more repeatable call, especially across six to ten units where symmetry, value stability, and remake control mattered more than one heroic incisal halo; but I have also seen single-central and minimal-prep anterior cases where E.max looked technically “correct” and still felt a little dead under mixed light. Why does the industry keep pretending one material can own every esthetic problem?
Artist Dental Lab’s own product structure quietly says the same thing. The site positions feldspathic veneers around hand-layered porcelain, enamel-like translucency, refined texture, and delicate anterior characterization, while its E.max veneer page frames lithium disilicate as the balanced route for strength, fit, shade performance, and single-to-multi-unit cosmetic workflows. That is not random. That is a case-selection map hiding in plain sight.
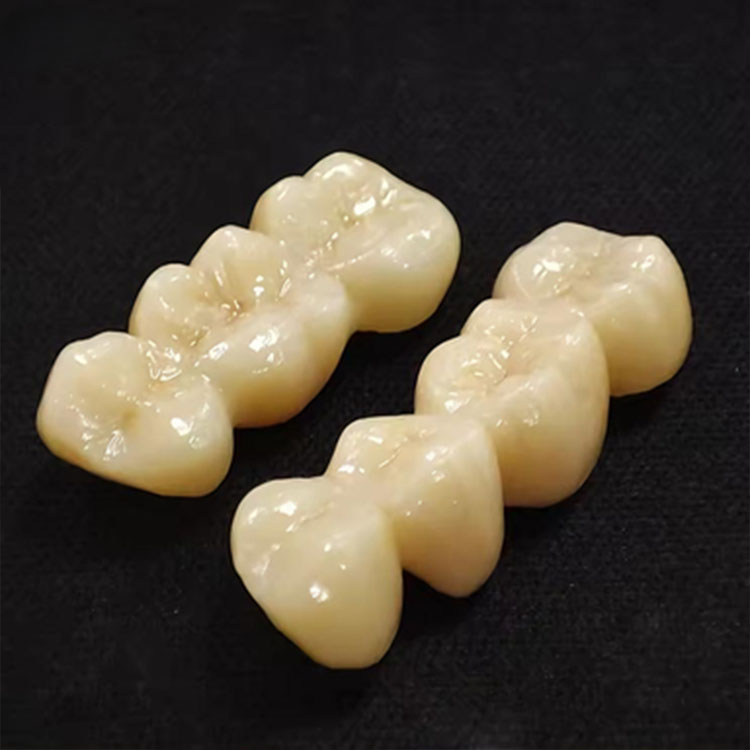
Feldspathic porcelain veneers make the most sense when the case is conservative, enamel-rich, anterior-only, and driven by optical invisibility rather than brute material security. I mean calm occlusion. Thin preparations. Friendly stump shade. A patient who wants “my teeth, but better,” not a Hollywood mask.
The best candidates are often the cases that do not look dramatic on a sales page:
A lateral peg-shape correction with enough enamel to bond cleanly.
A single central incisor where texture, halo, and line-angle behavior must match the natural neighbor.
A minimal-prep smile makeover where the clinician is adding volume, not hiding darkness.
A diastema closure where translucency and edge vitality matter more than blocking power.
A young-looking smile where overbuilt opacity would make the final result look expensive but fake.
But here is the hard truth: feldspathic veneers are not forgiving. They punish sloppy prep. They punish parafunction. They punish missing stump photos. They punish “just make it A1” prescriptions. And they really punish labs that no longer have true powder-liquid anterior artists.
That is why the layered E.max veneer workflow exists as a halfway house: lithium disilicate core, porcelain layering, more depth than monolithic E.max, and more mechanical margin than traditional feldspathic in many cases. Artist Dental Lab describes layered E.max as a lithium disilicate core with porcelain layering for depth, vitality, incisal effects, and premium anterior esthetics, which is exactly how I would frame it to a skeptical clinician.
The numbers do not support lazy tribalism.
A 2025 PubMed-indexed meta-analysis on ceramic laminate veneers reported pooled survival at about 10.4 years of 96.13% for feldspathic, 93.70% for leucite-reinforced glass ceramic, and 96.81% for lithium disilicate. Read that twice. The feldspathic vs Emax veneers fight is not a simple “old weak porcelain vs modern strong ceramic” story when cases are selected properly. It is closer than the brochures admit. Read the PubMed abstract here.
Another survival paper makes the more useful point: dentin exposure changes the game. A 2025 retrospective clinical study of 672 ceramic veneers in 189 patients followed for 1 to 15 years reported a cumulative 15-year estimated survival rate of 96%, with enamel-only cases at 96.7%, less than 30% dentin exposure at 95.3%, and more than 30% dentin exposure at 93.9%. Translation: the tooth substrate may matter more than your ceramic ideology. See the Wiley study page.
And yes, E.max has real engineering behind it. Ivoclar lists IPS e.max CAD at 530 MPa flexural strength and 2.11 MPa·m¹ᐟ² fracture toughness, with several translucency and shade options. That is why lithium disilicate veneers are often the cleaner call for moderate color change, multi-unit consistency, and cases where the operator needs a wider safety margin. Ivoclar’s IPS e.max CAD page gives the material data.
So no, feldspathic is not automatically “better.” It is better when the case lets it be better.
| Smile Makeover Factor | Better Suited to Feldspathic Veneers | Better Suited to E.max Veneers | My Blunt Take |
|---|---|---|---|
| Prep style | Minimal-prep, enamel-rich, additive cases | Standard veneer reduction, more controlled thickness | Feldspathic loves conservative enamel; E.max tolerates more workflow variability |
| Stump shade | Light, friendly, low masking demand | Moderate discoloration or value-control needs | Do not ask translucent porcelain to hide a dark problem |
| Unit count | 1–4 high-detail anterior units | 6–10 unit smile makeovers needing consistency | Multi-unit sameness usually favors lithium disilicate |
| Optical goal | Maximum enamel mimicry, halo, craze lines, micro-texture | Natural esthetics with stronger repeatability | Feldspathic wins the art contest only when the case is calm |
| Functional risk | Low parafunction, stable guidance | Higher control needs, broader clinical tolerance | Bruxers do not care about your romance with feldspathic |
| Lab dependency | Extremely high | High, but more systemized | Feldspathic quality is technician-dependent in a brutal way |
| Bonding demand | Adhesive bonding, enamel preservation essential | Adhesive bonding also essential | Material choice cannot rescue poor bonding |
| Best internal Artist Dental Lab match | hand-layered feldspathic porcelain veneers | standard E.max veneer indications or full E.max veneer consistency | Use the page that matches the risk, not the one with the prettiest promise |
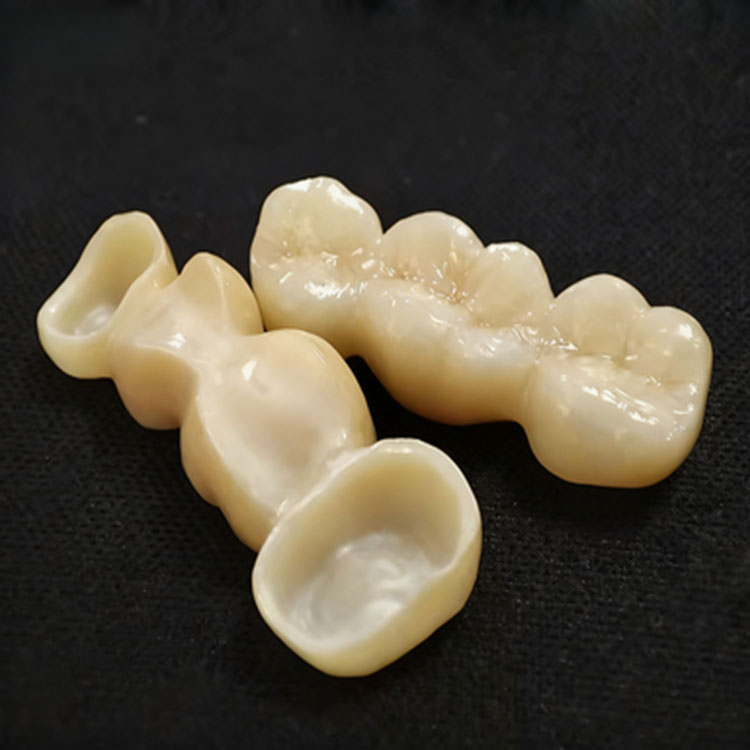
If the prep is mostly enamel and the dentist is adding shape, contour, or edge length rather than hiding severe discoloration, feldspathic porcelain can be the best veneer material for a natural smile makeover. The optical behavior is the point. You are not using feldspathic because it wins a strength chart. You are using it because it disappears.
This is where Artist Dental Lab’s feldspathic porcelain veneer positioning makes sense: high-end smile design, minimal-prep cosmetic cases, complex shade blending, delicate incisal effects, and customized texture. That is exactly the territory where feldspathic earns its fee.
A single central incisor is where cheap certainty goes to die.
E.max can work beautifully, especially layered E.max. But if the neighboring natural central has wild surface anatomy, translucent incisal edge behavior, subtle internal warmth, and a value shift that changes from window light to operatory light, feldspathic still has a seat at the table.
Would I use feldspathic for every central? No. But for the right central, with excellent photos, stump shade, facebow or digital bite context, and a ceramist who can actually layer, I would rather trust feldspathic than force a stronger ceramic into an optical job it was never born to dominate.
Younger enamel has a certain violence to it under light: brightness, depth, translucency, and surface irregularity all happening at once. Over-masking that with an opaque lithium disilicate result can make the smile look finished but not alive.
This is where cosmetic dentistry gets dishonest. Patients say they want white. What they really want is believable white.
Feldspathic veneers can preserve that illusion when the underlying tooth color cooperates. If the prep is light, the value target is controlled, and the patient is not asking for bathroom-tile opacity, feldspathic porcelain gives the ceramist more room to mimic enamel rather than just cover tooth structure.
For six, eight, or ten veneers, I usually lean toward E.max veneers or full E.max veneers unless the case is unusually disciplined. Why? Because repeatability beats poetry when every incisal edge, contact, value transition, and midline perception has to behave across the arch.
Artist Dental Lab’s full E.max veneer page emphasizes monolithic lithium disilicate, predictable fit, consistent strength, and efficient B2B cosmetic workflows. That is exactly the safer lane for many commercial smile makeovers.
If the case needs real masking, feldspathic becomes less charming. The more translucency you preserve, the more the stump shade gets a vote.
E.max, especially selected in the right translucency and thickness, gives the clinician and lab better control over value and chroma. That does not mean E.max always looks better. It means it gives you more room to manage a compromised starting point.
This is where I would connect the treatment plan to the lab’s E.max veneer material pathway rather than pretending feldspathic can solve every discoloration case with enough artistry.
Some teeth should not be veneers. There. I said it.
When the tooth has large old composite, cracks, endodontic history, severe wear, heavy dentin exposure, or a structural problem hiding behind a cosmetic request, the honest answer may be an E.max crown or another full-coverage restoration. Artist Dental Lab’s guide on the indication boundary between E.max veneers and E.max crowns is the kind of internal link I would want in this article because it forces the reader to stop treating veneers like a fashion category.
The veneer market has been polluted by price-first marketing. That pressure leaks upward into legitimate dentistry too: patients ask for “veneers,” influencers sell outcomes, and some providers start choosing materials like they are picking filters.
The Associated Press reported in October 2024 that dentists often charge $1,000 to $2,000 per tooth for veneers, while unlicensed “veneer techs” were advertising full sets for $4,000 to $5,000 and performing dental work illegally. The same report noted that all U.S. states require dental work, including veneers, to be performed under licensed dental supervision. Read the AP report on fake veneer providers.
That matters because material selection is not branding. It is diagnosis, consent, risk control, and documentation. The moment a smile makeover case becomes “just pick feldspathic or E.max,” the case has already been dumbed down.
And bonding is not a footnote. For E.max veneers, Artist Dental Lab’s standard bonding protocol for E.max veneers correctly centers the discussion on hydrofluoric-acid etching, silane, tooth conditioning, resin cement, and contamination control. The CDC’s hydrogen fluoride guidance notes that skin exposure may not cause immediate visible damage and that visible injury can be delayed 12 to 24 hours, which is a useful reminder that “routine” adhesive steps still require respect. CDC hydrogen fluoride safety guidance.
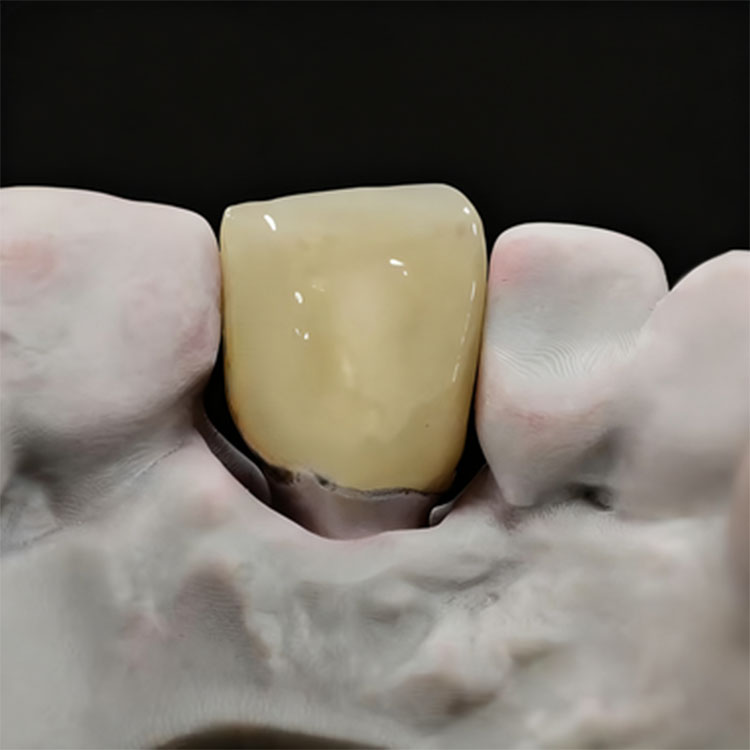
Feldspathic veneers are better suited to smile makeover cases with strong enamel preservation, light stump shades, low functional risk, minimal-prep design, and high anterior esthetic demands where translucency, incisal halo, surface texture, and enamel-like light behavior matter more than broad mechanical tolerance or multi-unit production consistency. These are usually premium anterior cases, not routine masking cases.
In practical terms, I would consider feldspathic first for one to four visible anterior veneers, especially single-central matching, diastema refinement, peg lateral correction, mild shape changes, and additive smile design where the patient wants natural character instead of a uniform cosmetic shell.
E.max veneers are often better than feldspathic veneers for full smile makeovers when the case involves six or more units, moderate shade correction, stricter value control, higher functional uncertainty, or a need for repeatable fit and strength across the arch rather than maximum hand-layered optical nuance in one or two teeth. That is the commercial reality.
I still like feldspathic for selected anterior artistry, but when the case becomes a full-arch esthetic workflow, lithium disilicate veneers often give the dentist, lab, and patient a cleaner risk profile.
Feldspathic porcelain is generally more technique-sensitive and mechanically less forgiving than lithium disilicate, while E.max-type lithium disilicate offers higher strength and broader clinical tolerance; however, survival data for properly selected veneer cases show both material categories can perform well when bonding, enamel preservation, occlusion, and case selection are controlled. The weak link is often the plan.
So I would not call feldspathic “bad.” I would call it less forgiving. There is a difference, and that difference is expensive when the wrong case gets romanticized.
Dentists should send STL or IOS scans, opposing and bite records, stump shade, final shade target, retracted photos, full-face smile photos, prep-depth notes, margin design, mock-up or provisional references, occlusal risk notes, and specific requests for value, translucency, incisal halo, craze lines, and surface texture. Without those records, feldspathic becomes guesswork.
That is also why I would send complex anterior cases only to a lab that can explain material choice clearly. Artist Dental Lab’s guide on evaluating premium anterior esthetics is useful because it treats material judgment, shade discipline, documentation, and remake control as one connected workflow.
A dentist should avoid feldspathic veneers when the case has dark stump shades, heavy parafunction, poor enamel support, major dentin exposure, large restorations, endodontic history, severe wear, or a multi-unit demand for high consistency that exceeds what hand-layered porcelain can predictably control. Beauty does not excuse bad indication selection.
In those cases, E.max veneers, layered E.max veneers, full E.max veneers, E.max crowns, or even zirconia-based options may be more honest depending on the tooth structure and risk profile.
Here is my final position: feldspathic veneers are better than E.max only in the cases that deserve feldspathic. That means conservative enamel, friendly stump shade, low occlusal risk, and a visual target that demands enamel mimicry more than systemized strength.
For everything else, stop being sentimental.
If the smile makeover needs six to ten units, tighter value control, stronger masking, more predictable fit, or less dependence on a master ceramist’s hand, use the E.max veneer, full E.max veneer, or layered E.max veneer pathway instead of forcing feldspathic into a job it was not meant to carry.
If you are planning a premium anterior case, send the lab real records: stump shade, pre-op photos, prep photos, smile line, midline, occlusion, desired texture, and the actual reason you think feldspathic is justified. Then ask for a material recommendation before production.
The CTA is simple: before your next smile makeover, audit the case by enamel, stump shade, unit count, and functional risk. If the case is quiet and optical, choose feldspathic with discipline. If the case is broader, darker, heavier, or less perfectly documented, choose E.max with no apology.