


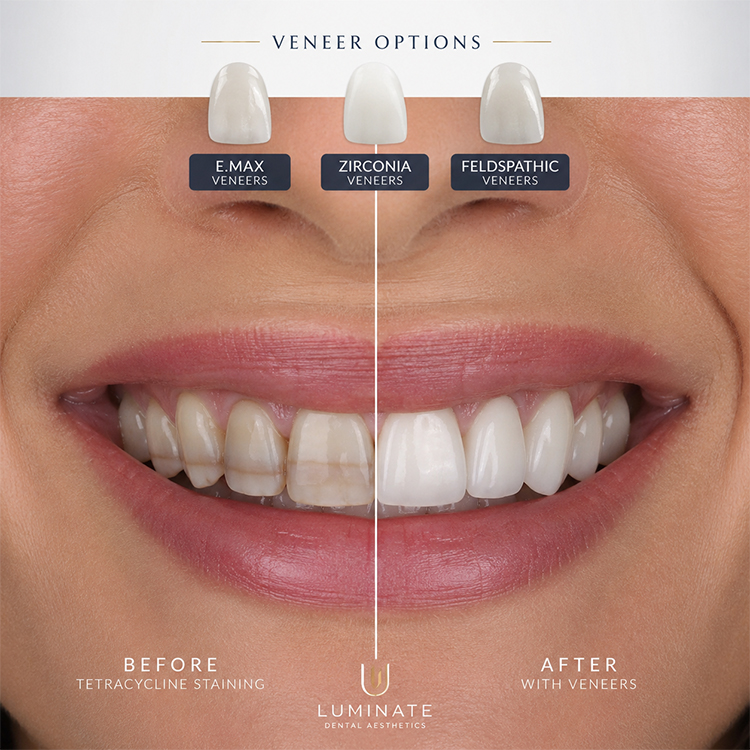
Tetracycline-stained teeth veneers are not a simple beauty purchase. The real decision sits at the intersection of masking power, enamel bonding, stump shade, ceramic thickness, cement value, occlusion, and whether the lab can control the final result under ugly clinical conditions.
Marketing lies softly.
When a patient walks in with gray-brown banding from tetracycline exposure, the wrong question is “Which veneer looks the most natural?” because natural-looking ceramic means nothing if the substrate is screaming through 0.4 mm of porcelain, the stump shade was never recorded, and the cement was chosen like an afterthought. So why do so many treatment plans still start with a material name?
Tetracycline staining is not coffee stain. It is intrinsic discoloration, often embedded during tooth development. The CDC notes that older tetracycline-class antibiotics have been linked to permanent tooth staining and enamel hypoplasia when used in children under 8; a warning label was added to tetracycline-class antibiotics in 1970 for that reason. See the CDC’s own background on doxycycline and tooth staining.
That matters because best veneers for tetracycline stained teeth is not a one-material answer. It is a masking problem, a bonding problem, and sometimes a consent problem. I’ll say the quiet part: mild tetracycline staining can make feldspathic look heroic; severe banding can make ultra-translucent ceramics look naïve.
For a lab workflow, I would anchor the case around Artist Dental Lab’s E.max veneer workflow when the case needs lithium disilicate predictability and shade control. Their E.max veneer page positions the material as lithium disilicate for natural translucency, reliable strength, precise fit, conservative-to-multi-unit cases, and moderate color improvement.
But moderate is the word that should make everyone pause.
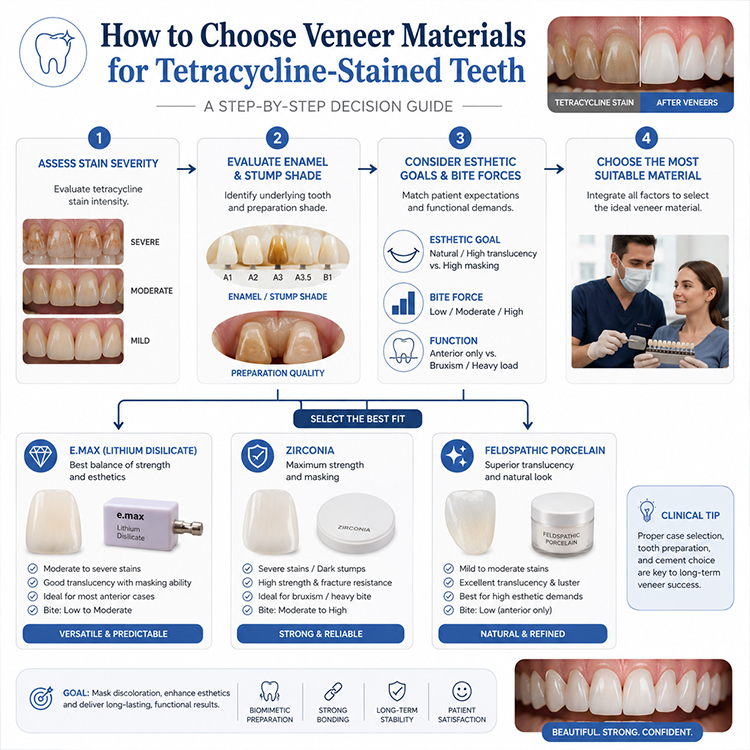
E.max, zirconia, and feldspathic do not solve the same problem. They can all be sold as premium. They should not all be prescribed as premium.
E.max veneers are lithium disilicate ceramics, often discussed chemically as Li₂Si₂O₅. In tetracycline cases, I like E.max because it gives the clinician and lab a better balance of strength, esthetics, thickness control, and masking strategy than a purely romantic “thin porcelain” plan.
Artist Dental Lab describes its standard lithium disilicate E.max veneers as a balance of strength and esthetic translucency, with case-dependent indications including anterior and premolar veneers, shape correction, moderate color improvement, and esthetic rehabilitation planning.
Here is the hard truth: E.max veneers for tetracycline stains are usually safest when the clinician accepts that the restoration may need more opacity, more thickness, or a smarter cement value than a social-media veneer case.
Layered E.max is where the artistry gets seductive. A lithium disilicate core plus porcelain layering can create depth, halo, incisal translucency, warmth, and lifelike texture. Artist Dental Lab frames its layered E.max veneer for high-end anterior smile makeovers requiring detailed characterization, nuanced translucency, and lifelike surface texture.
Great.
Also dangerous.
If the stump shade is dark and the case needs heavy masking, the ceramist is no longer just creating beauty; they are negotiating with opacity, brightness, and thickness. Push too translucent and the gray returns. Push too opaque and the case starts to look like bathroom tile. What wins then?
Control wins.
Zirconia is zirconium dioxide, ZrO₂. It is the material many clinicians reach for when they hear “dark tooth,” “bruxer,” or “high strength.” I get it. But zirconia veneers for tetracycline teeth are not automatically better just because zirconia is tougher.
Artist Dental Lab’s zirconia veneer page positions it for high-strength cosmetic cases, higher functional demands, added fracture resistance, and challenging bite conditions with appropriate planning.
That is a narrow indication, not a blank check.
Zirconia can help when durability dominates the risk profile. But in high-smile-line anterior cases, especially where incisal vitality and enamel-like fluorescence matter, zirconia can be too optically blunt unless the system, thickness, staining, and finishing are handled with discipline.
Feldspathic veneers are still the most poetic option when the prep is conservative, enamel is abundant, the stain is mild-to-moderate, and the patient is paying for light behavior rather than just whiteness. Artist Dental Lab describes its feldspathic veneer as hand-layered porcelain for enamel-like translucency, refined surface texture, premium anterior esthetics, complex shade blending, and delicate incisal effects.
That is exactly where feldspathic earns its fee.
But severe tetracycline staining? That is where feldspathic can become a trap. The same translucency that makes it beautiful can betray the case when gray-brown banding sits underneath.
A 2005 clinical evaluation followed 546 tetracycline-stained teeth treated with porcelain laminate veneers and reported excellent marginal adaptation in 99% of veneers, less than 1% rebonding in the first six months, stable color, and broad patient satisfaction after one year. That is not Instagram evidence. That is actual recall data from a large tetracycline veneer cohort: Clinical evaluation of 546 tetracycline-stained teeth treated with porcelain laminate veneers.
A 2017 clinical case report on severe tetracycline dental discoloration used conventional feldspathic ceramic veneers, showing that feldspathic can work even in a difficult esthetic case when planning, preparation, opacity control, and bonding are handled properly: Severe tetracycline dental discoloration restored with feldspathic ceramic veneers.
Another clinical report described minimally invasive management of tetracycline staining in two cases with different severities, which is exactly how this topic should be discussed: not as “which ceramic is best,” but as “how severe is the substrate problem?” See Minimum Intervention in Managing Two Cases of Tetracycline Staining.
And if we widen the lens beyond tetracycline cases, the NCBI Bookshelf summary of a systematic review found feldspathic porcelain veneer survival at 95.7% at 5 years, with a 10-year estimate that may approach 95.6% when bonded to enamel, while warning that heterogeneity across studies affects interpretation. Read the NCBI summary: survival of feldspathic porcelain veneers over 5 and 10 years.
So no, feldspathic is not “weak.” That lazy statement needs to die.
The real question is whether the case gives feldspathic the enamel, thickness, shade control, and functional protection it demands.
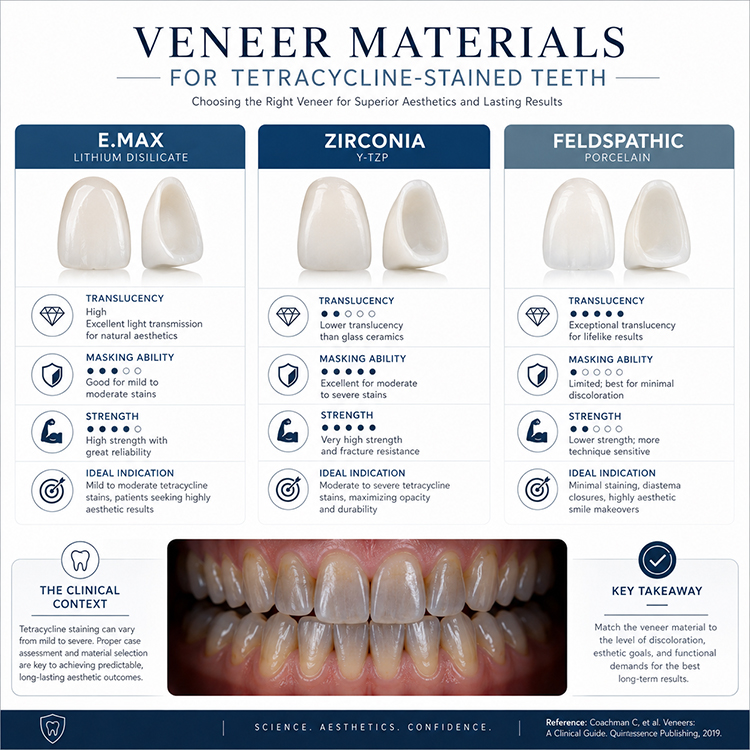
| Decision Point | E.max / Lithium Disilicate Veneers | Zirconia Veneers | Feldspathic Veneers |
|---|---|---|---|
| Core material logic | Li₂Si₂O₅ glass-ceramic; balance of strength and translucency | ZrO₂ ceramic; durability-first, often monolithic | Hand-layered porcelain; maximum enamel-like optical nuance |
| Best tetracycline indication | Mild-to-moderate stains; moderate masking; multi-unit consistency | Darker substrates with functional risk, when esthetics can be managed | Mild stains, conservative preps, high-end anterior texture |
| Weak spot | Can look too bright or flat if opacity is overused | Can look less vital in the anterior zone if handled bluntly | Can fail esthetically when asked to mask severe gray banding too thin |
| Lab dependency | High | High | Very high |
| Stump shade importance | Mandatory | Mandatory | Non-negotiable |
| Cement shade importance | High | Case-dependent but still important | Very high |
| My blunt take | Best default for many tetracycline-stained teeth veneers | Strong answer for selected high-risk cases, not beauty-first cases | Best-looking material only when the biology and stain severity allow it |
First, grade the stain.
A patient with faint yellow-gray discoloration and intact enamel is not the same case as a patient with dark cervical bands, old composites, parafunction, and unrealistic B1 expectations, and pretending those cases belong in the same material bucket is how remakes are born. Would you rather impress the patient at the consult, or still like the result at seating?
For mild tetracycline staining, feldspathic or layered E.max can be stunning. For moderate staining, I would usually start the conversation around E.max because it gives the team more room to manage value and translucency. For severe staining, I become suspicious of thin veneers, aggressive “no-prep” promises, and any plan that does not include stump shade photography.
Second, protect enamel.
This is where the internet gets sloppy. Veneers are sold as conservative, but they are still irreversible. The AP reported that veneers commonly cost $1,000–$2,000 per tooth, involve removing some enamel, are generally not covered by insurance, and typically last 5 to 15 years before needing replacement. Their reporting also flagged the illegal “veneer tech” trend and the risks of unlicensed dental work: AP on fake dentists and cheap veneers.
Third, demand records.
For a tetracycline-stained case, I would not send a lab only “A1, natural look.” That is malpractice by laziness. Send STL scans, prep/opposing/bite files, stump shade, retracted photos, smile photos, polarized photos if possible, prep depth notes, occlusal risk notes, and a written target for value, chroma, translucency, and incisal edge behavior.
Artist Dental Lab’s own anterior comparison guide says clinicians should send full photos, stump shade, STL files, occlusion notes, and the esthetic target when choosing among E.max, layered E.max, feldspathic, and zirconia veneer workflows.
I agree with that completely.
Dental spending is not a small corner of healthcare anymore. The ADA Health Policy Institute reported that U.S. national dental expenditure reached $189 billion in 2024, representing 3.6% of total health expenditure, with inflation-adjusted dental spending rising 4% from 2023 to 2024. See the ADA’s National Dental Expenditures, 2024.
That money pulls in serious clinicians.
It also pulls in amateurs.
The ADA warned in May 2024 that “veneer technicians” offering services on social media may cause damaging complications, and that dental procedures altering teeth, gums, or jaws without dentist supervision can cause irreversible harm. Read the ADA warning on veneer techs and dental damage.
Here is my unpopular opinion: tetracycline cases should never be sold as quick cosmetic upgrades. They are prosthetic masking cases with esthetic ambitions. That means the dentist, lab, and patient all need to understand the tradeoff between reduction, opacity, naturalness, longevity, and future replacement.
If you are a clinic or lab buyer comparing vendors, use Artist Dental Lab’s contact and trial case page only after you have the records ready: the site itself lists typical requests including B2B price list, first trial case, veneers and smile design, full-arch and implants, and OEM/private-label work.
I would choose E.max veneers for tetracycline stains when the case is mild-to-moderate, the patient wants a brighter smile, the prep allows enough thickness, and the team needs consistent value across 6, 8, or 10 anterior units. This is the rational middle lane.
Use full E.max veneers when consistency and fit matter more than hand-built drama; Artist Dental Lab positions this monolithic option for predictable fit, consistent strength, natural translucency, single units, and multi-unit smile enhancement.
Layered E.max belongs in the visible esthetic zone when the patient has a high smile line, good records, enough reduction, stable occlusion, and a realistic shade goal. The porcelain layer can buy depth and character. It can also buy variability.
So I would use it selectively.
Zirconia veneers make sense when fracture resistance and functional risk are real, not imagined. Bruxism, compromised bite design, or high-load situations may push the case toward zirconia. But do not pretend zirconia is automatically the best answer for ceramic veneers for stained teeth. Stronger is not always prettier.
Feldspathic is still the premium answer for conservative anterior esthetics when the case lets the ceramist use translucency rather than fight it. For mild tetracycline discoloration, diastema closure, shape correction, incisal effects, and enamel-like texture, feldspathic can embarrass heavier materials.
For severe gray-brown banding, I become much less romantic.
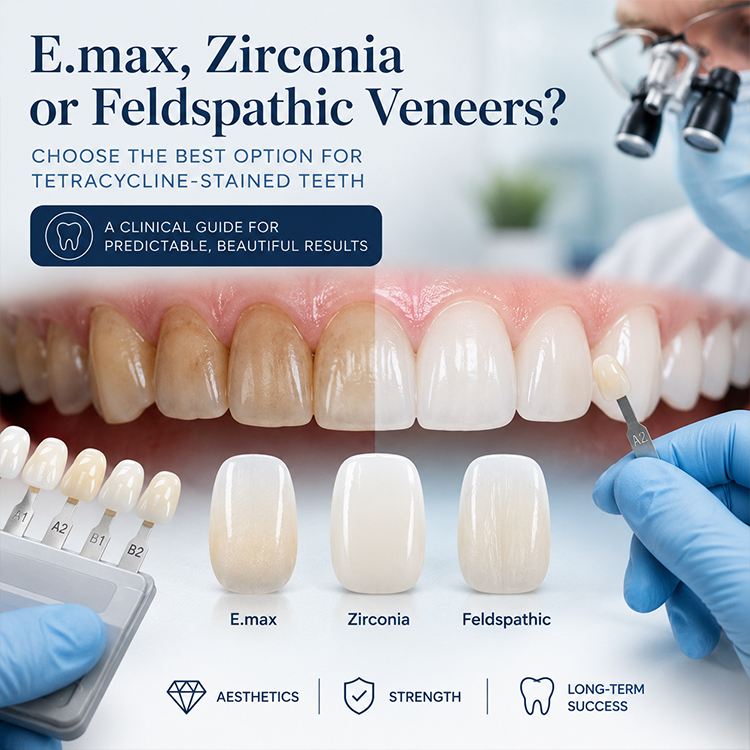
The best veneers for tetracycline-stained teeth are ceramic restorations selected by stain severity, stump shade, enamel availability, reduction space, and esthetic goal, with E.max often serving as the balanced default, zirconia reserved for higher functional risk, and feldspathic used when conservative enamel bonding and natural light behavior matter most.
In mild cases, feldspathic or layered E.max may create the most natural result. In moderate cases, lithium disilicate veneers for dark teeth usually give better control. In severe cases, the dentist may need more opacity, deeper preparation, or even crowns if veneers cannot mask the substrate responsibly.
E.max veneers are good for many tetracycline stains because lithium disilicate offers a practical blend of translucency, strength, adhesive compatibility, and masking flexibility, but the result depends heavily on ceramic thickness, ingot or block opacity, cement shade, stump shade documentation, and the patient’s tolerance for a slightly brighter restoration.
I would not call E.max magic. I would call it controllable. That is a compliment in tetracycline cases, because control beats romance when the tooth underneath is dark.
Zirconia veneers can be better than E.max for selected dark-tooth cases when fracture resistance, functional load, or masking demand outweigh the need for maximum translucency, but zirconia is not automatically superior in anterior esthetics because it can look less enamel-like if material thickness, finishing, and shade design are not handled carefully.
My view is simple: choose zirconia when function forces the conversation. Do not choose it just because “dark tooth” sounds scary.
Feldspathic veneers can work for tetracycline discoloration when the stain is mild-to-moderate, enamel bonding is strong, preparation is conservative but adequate, and the ceramist can manage opacity without losing natural translucency; however, severe gray-brown banding may exceed what thin feldspathic porcelain can mask predictably.
Feldspathic is beautiful because it lets light move. That same feature becomes a liability when the underlying tooth color is too aggressive.
A dentist should send the lab STL scans, opposing scans, bite records, stump shade, standard shade, retracted photos, smile photos, prep depth notes, occlusion notes, desired value, translucency target, incisal characterization preferences, and any mock-up or wax-up reference before choosing E.max, zirconia, or feldspathic veneers.
Without those records, the lab is guessing. And when the substrate is tetracycline-stained, guessing is expensive.
Do not choose E.max, zirconia, or feldspathic because a sales page made the material sound elite. Choose it because the stain severity, enamel, stump shade, reduction, occlusion, cement strategy, and lab workflow all point in the same direction.
For most tetracycline-stained teeth veneers, my default starting point is E.max or layered E.max. For high-risk functional cases, zirconia earns a serious look. For conservative, enamel-rich, mild-discoloration anterior cases, feldspathic still has the most beautiful ceiling.
But the case decides.
If you are planning a tetracycline-stained veneer case, start by collecting stump shade photos, retracted images, smile-line photos, STL files, and bite records, then compare Artist Dental Lab’s E.max veneer, layered E.max veneer, zirconia veneer, and feldspathic veneer workflows before you prescribe the material. Then submit a trial case through the Artist Dental Lab contact page with the records that actually let the lab make a defensible recommendation.