


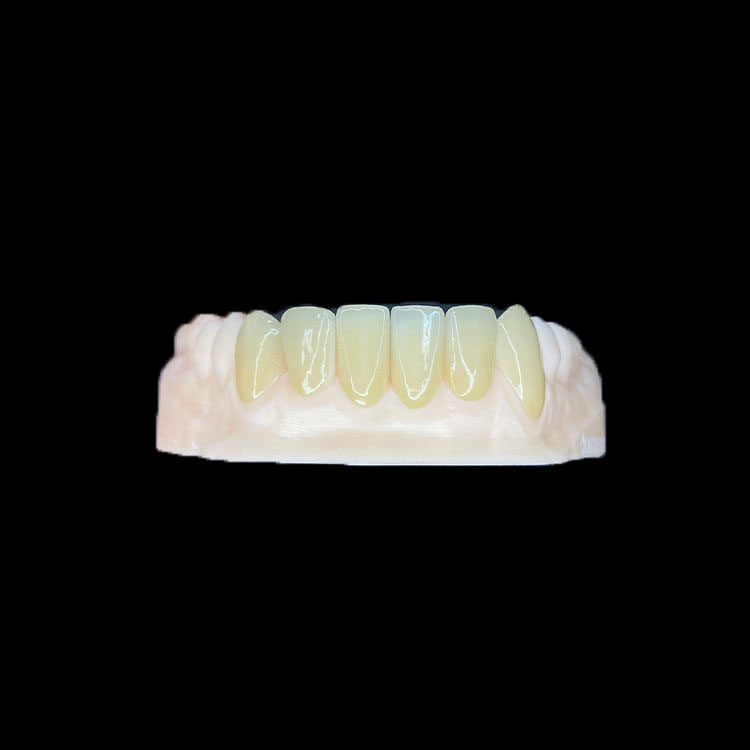
Multi veneer cases do not fail because the dentist “missed beauty.” They fail because the midline was not owned early, the symmetry was judged too late, and the lab received poetry instead of usable data.
Patients notice drift.
And in multi veneer cases, that drift rarely starts at cementation; it usually starts when the clinician accepts a casual smile photo, vague “match the mock-up” language, and a lab prescription that never names the facial midline, dental midline, incisal cant, gingival display, or the patient’s asymmetrical lip dynamics in measurable terms. Why are we still pretending symmetry appears at delivery?
Here is my hard rule: the veneer midline must be diagnosed before material selection, before reduction, and absolutely before anyone starts arguing about whether the case should be standard E.max veneers, full E.max veneers, layered E.max veneers, or feldspathic veneers. Artist Dental Lab’s own product structure makes the split obvious: standard E.max is positioned for balanced single-to-multi-unit cases, full E.max for predictable fit and consistency, layered E.max for higher anterior characterization, and feldspathic for enamel-like translucency and micro-texture.
That is not just catalog organization. That is risk mapping.
The uncomfortable part? Midline and dental veneer symmetry are not purely lab problems. They are shared failures when the dentist sends insufficient records and the lab “beautifies” the case without knowing which reference line owns the final result.
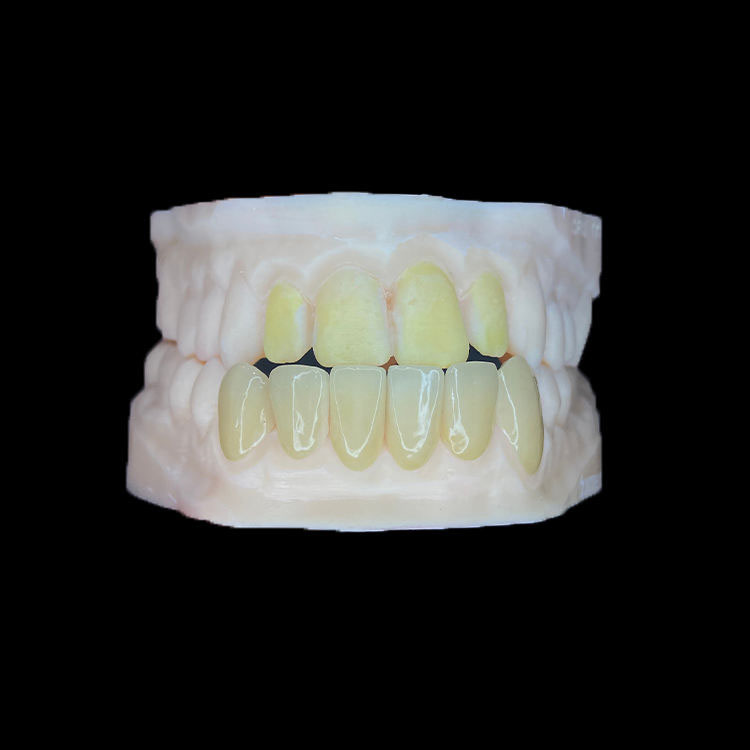
A classic esthetic perception study by Kokich Jr. and colleagues found that a maxillary midline deviation of 4 mm was needed before orthodontists rated the smile significantly less esthetic, while another study available through PubMed investigated how orthodontists and young laypeople perceive dental-to-facial midline discrepancies. More recent open-access work found that laypersons could perceive upper dental midline deviations of 1 mm or more when adjacent smile structures were included. Kokich Jr. et al. on PubMed, Johnston et al. on PubMed, and Ferreira et al. on PMC are worth reading before anyone waves off a 1–2 mm discrepancy as “clinically acceptable.”
Small numbers matter.
But the real danger is that clinicians often quote those thresholds as if every patient sees the same face, under the same lip mobility, in the same lighting, with the same obsessive post-op mirror behavior. They do not. The patient who paid for eight cosmetic dentistry veneers is not judging the case like a journal reviewer. They are zooming in on iPhone photos at 11:43 p.m.
So I would treat the 1 mm mark as a planning warning, not a panic point. I would treat 2 mm as a meeting. And I would treat 3–4 mm as a consent problem unless the patient already understands the skeletal, orthodontic, periodontal, or restorative compromise.
Before touching enamel, I want five records:
Then I want three reference lines: facial midline, maxillary dental midline, and planned restorative midline. They do not always match. Fine. But they must be named.
If the planned restorative midline is being cheated to improve the smile, say it. If the case is following the philtrum instead of the existing centrals, say it. If the lower midline is irrelevant to the patient’s visible smile, say it. Silence is where remakes breed.
Pretty words are useless.
A lab cannot maintain midline and symmetry in multi-veneer cases from “Hollywood smile, natural, bright but not fake.” That kind of prescription is not communication; it is a wish list with a shade tab attached.
What I want to see in the lab note is almost embarrassingly specific:
| Planning Variable | What to Record | Why It Matters in Multi Veneer Cases |
|---|---|---|
| Facial midline | Philtrum, nose bridge, chin axis, interpupillary reference | Prevents the dental midline from being judged in isolation |
| Dental midline | Existing central-incisor contact and proposed final contact | Shows whether the case is correcting or disguising asymmetry |
| Incisal plane | Smile photo plus horizontal reference | Prevents a straight midline with a tilted edge |
| Central dominance | Width/length ratio of 8 and 9 or 11 and 21 | Controls whether one central becomes the “fat tooth” |
| Gingival asymmetry | Tissue height, zeniths, recession, black triangles | Stops ceramic from being blamed for periodontal limits |
| Material choice | E.max, full E.max, layered E.max, feldspathic, zirconia | Determines how much optical freedom and workflow risk the case carries |
This is where Artist Dental Lab’s client-case workflow is relevant. Their case page describes examples built around challenge, solution, and measurable outcomes, including veneers-focused esthetic lines, standardized shade communication, photography protocols, shorter case times, and improved patient satisfaction with color, translucency, and contour.
I like that framework because it forces accountability. Not romance. Accountability.
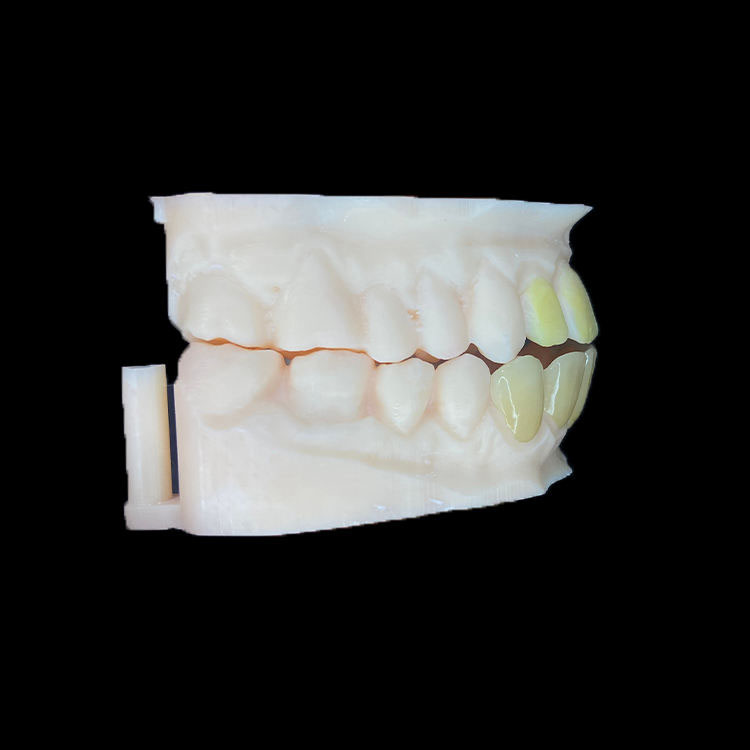
Let’s say the quiet part out loud: layered ceramics are not automatically better for dental veneer symmetry.
Full E.max can be the smarter choice for many six-, eight-, or ten-unit multi veneer cases because monolithic lithium disilicate reduces interpretive variation across units. Artist Dental Lab describes its full E.max veneer as monolithic lithium disilicate, optimized for predictable fit, consistent strength, shade control, stump-shade photos, clean margins, contact stability, and multi-unit cosmetic consistency.
Layered E.max earns its keep when the case needs incisal translucency, halo, internal characterization, and custom surface texture. Artist Dental Lab’s layered E.max veneer page asks for STL scans, shade and stump shade, retracted and smile photos, wax-up or mock-up references, midline and smile-line notes, and surface texture preferences. That list tells you the truth: the more premium the optical target, the more punishing weak records become.
Feldspathic porcelain is still the snob’s answer when enamel-like light behavior and micro-texture matter more than production speed. But I would not throw feldspathic at every multi veneer smile design just because the word sounds artisanal. In a broad case with uneven prep depth, dark stump shade, and a patient demanding uniform value, feldspathic can become a beautiful way to manufacture inconsistency.
The material is not the hero. The workflow is.
Ivoclar lists IPS e.max CAD with 530 MPa flexural strength and 2.11 MPa·m¹ᐟ² fracture toughness, which helps explain why lithium disilicate remains such a dominant ceramic family for bonded esthetic dentistry. Ivoclar’s IPS e.max CAD data supports the mechanical side of the conversation, but strength does not center a midline, fix a cant, or rescue a lazy prep guide.
Cementation is not cleanup. It is the final test of whether the case was actually controlled.
In anterior veneer case planning, I prefer a center-first logic: seat the two centrals first, verify midline, incisal edge, contact pressure, value, and cant, then move laterally in a controlled sequence. Artist Dental Lab’s own article on the most efficient cementation sequence for multiple veneers makes a similar point: material choice changes workflow headaches, but it does not erase sequence discipline.
Here is the sequence I would not skip:
Check midline, incisal edge, embrasure symmetry, central width, and canine line before cement shade distracts everyone.
Teeth dehydrate fast. A veneer that looks too high-value after long isolation may not be wrong; the tooth may just be dry.
The centrals control the case. If the central contact is wrong, the rest of the smile becomes organized around a lie.
Seat laterals and canines only after the central-incisor relationship is stable. Do not chase speed at the cost of the midline.
Take a straight-on smile photo before the patient leaves. Not because photos are marketing. Because photos catch what adrenaline hides.
I am going to be blunt. The veneer market has a supervision problem.
The American Dental Association issued a May 14, 2024 statement warning the public about “veneer technicians,” saying unsupervised dental treatment from unlicensed people may cause damaging complications and that procedures altering teeth, gums, or jaws without dentist supervision may cause irreversible harm. The ADA also named risks including infection, nerve damage, and choking hazards.
The Associated Press later reported that dentists were warning about unlicensed veneer providers on social media, with some advertising low-cost full sets, while typical dentist fees were reported around $1,000 to $2,000 per tooth and veneers were described as lasting roughly 5 to 15 years before replacement.
Why mention this in an article about veneer midline and symmetry?
Because the same market that tolerates “veneer tech” nonsense also tolerates sloppy planning wrapped in luxury language. Different degree. Same disease. A professional multi veneer case should have diagnosis, consent, material logic, lab communication, and a controlled delivery sequence. Anything less is cosmetic gambling.
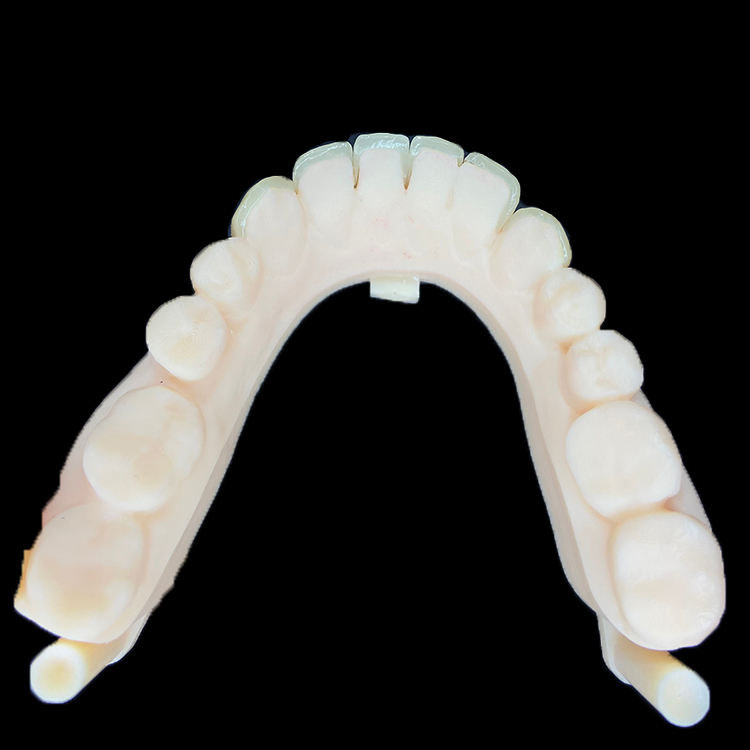
The best way to maintain midline in multi veneer cases is to define the facial midline, existing dental midline, and proposed restorative midline before preparation, then communicate those references to the lab with full-face photos, retracted views, STL scans, stump shade, mock-up records, and clear center-first cementation instructions.
After that, protect the plan. Do not let the lab “improve” the centrals without permission. Do not let the patient choose a whiter shade that destroys value harmony. And do not bond laterals before the central-incisor contact and incisal edge have been verified.
Acceptable dental midline deviation in veneers depends on facial symmetry, smile display, lip mobility, patient expectations, and whether the discrepancy is visible in full-face context, but many clinicians treat 1 mm as noticeable in sensitive cases and 2 mm or more as something that should be discussed before final bonding.
The mistake is using a journal threshold as an excuse. A low-smile patient may tolerate more. A high-smile patient with eight veneers and a ring light may tolerate less.
Full E.max is often better for multi veneer symmetry when repeatability, value control, and unit-to-unit consistency matter most, while layered E.max is better when the case needs higher anterior characterization, incisal translucency, halo effects, warmth control, and hand-built surface texture.
My bias is simple: choose full E.max when the case needs discipline across 6–10 units. Choose layered E.max when the case earns that extra optical complexity. Choose feldspathic only when the esthetic demand and clinical conditions justify the added technique sensitivity.
The lab should receive STL scans, opposing scan, bite record, full-face smile photos, retracted photos, shade and stump-shade records, mock-up or wax-up references, facial midline notes, smile-line notes, incisal-edge instructions, surface texture preferences, and a clear statement of whether the final midline is being corrected or intentionally compromised.
That last part matters. “Correct the midline” and “make it look centered in the smile” are not always the same instruction.
Symmetrical veneer cases still look fake when the teeth are mathematically even but biologically wrong: too uniform in value, too flat in texture, too identical in incisal embrasures, too wide in the laterals, too opaque at the edge, or too disconnected from the patient’s gingival architecture and lip movement.
Perfect symmetry can look artificial. Controlled asymmetry often looks alive. The trick is knowing which asymmetry to preserve and which asymmetry to eliminate.
Before prescribing your next multi veneer case, run a 10-minute midline audit: mark the facial midline, existing dental midline, planned restorative midline, incisal plane, central width ratio, gingival asymmetry, and material risk profile.
Then send the case to a lab that can discuss symmetry like a clinical problem, not a beauty slogan. For repeatable multi-unit work, compare E.max veneers with full E.max veneers. For premium anterior characterization, compare layered E.max veneers with feldspathic veneers. And when the case demands a structured B2B discussion, start with Artist Dental Lab’s contact page instead of sending a vague prescription and hoping ceramic can fix planning.