



E.max vs zirconia is not just a material debate. It is a surface-treatment problem. Get the intaglio protocol wrong, and the prettiest restoration in the box turns into a remake waiting for a calendar date.
Different chemistry. Different rules.
E.max is a glass-ceramic based on lithium disilicate, so its internal surface wants micromechanical etching and silane chemistry, while zirconia is an oxide ceramic with no glass phase at all, which means hydrofluoric acid does not do the same job and an MDP-based approach becomes the real bonding play. Why do so many clinicians still act like one bottle can solve both?
I’ll say the quiet part out loud.
A lot of “bonding failures” are not mysterious failures. They are protocol failures dressed up as bad luck, because once you confuse a silica-containing ceramic with a polycrystalline oxide ceramic, you start making the wrong surface roughness, the wrong chemical pretreatment, and the wrong cementation decisions before the case ever touches the tooth.
According to Ivoclar’s pretreatment guidance, glass-ceramics including lithium disilicate are conditioned by hydrofluoric acid etching followed by a silane-containing primer, while zirconium oxide is conditioned by aluminum-oxide sandblasting and then an MDP-containing primer because silane alone does not work on a material with no glass particles. That is the whole fight in one sentence.
Glass phase matters.
For lithium disilicate, the point of hydrofluoric acid is to create a retentive etched surface inside the restoration, and the point of silane is to couple that etched ceramic to the resin matrix, which is why the lithium disilicate bonding protocol keeps coming back to the same old sequence even when brands try to make it sound exotic. Isn’t that simpler than the marketing copy?
If your case is built around anterior-focused E.max crowns, Artist Dental Lab already frames them around translucency, esthetic-zone use, and resin-based or adhesive cementation protocols, which is the correct signal to send because E.max becomes more predictable when the adhesive workflow is not treated like an afterthought.
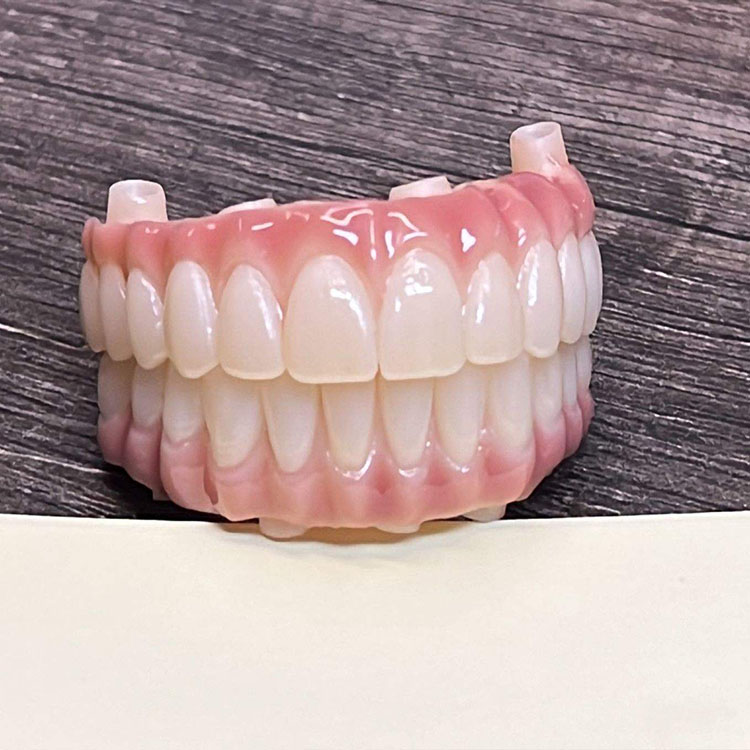
No glass. No free pass.
Zirconia does not give you the etched glass-ceramic interface that E.max does, so the zirconia bonding protocol shifts toward controlled airborne-particle abrasion and chemical adhesion with 10-MDP, short for 10-methacryloyloxydecyl dihydrogen phosphate, rather than pretending HF and silane can magically create chemistry that the substrate simply does not support. Why fight the material instead of reading it? (Ivoclar)
That is also why a serious lab separates full-contour multilayer zirconia crowns and bridges from layered zirconia crown cases for the smile zone: one is sold around monolithic function and reduced chipping risk, the other around a zirconia core plus porcelain layering for better depth and surface detail. Same family. Different risk profile.
Here is the version I wish more teams used before they touched a primer.
| Clinical step | E.max / lithium disilicate | Zirconia | What goes wrong when people mix them up |
|---|---|---|---|
| Material type | Glass-ceramic | Oxide ceramic | The wrong chemistry gets selected from step one |
| Intaglio activation | Hydrofluoric acid etch | Aluminum-oxide air abrasion / sandblasting | Retention and surface energy get mismanaged |
| Chemical pretreatment | Silane primer | MDP-containing primer | Silane-only zirconia protocols fall flat |
| Typical cement logic | Often adhesive or resin-based, especially for thin esthetic work | Case-dependent; conventional or resin depending on retention and protocol | Cement choice gets made before substrate prep is correct |
| Biggest operator mistake | Overlooking etch-and-silane discipline | Treating zirconia like glass-ceramic | Debonding gets blamed on the lab instead of the protocol |
That table is not theory. It is the practical split described in Ivoclar’s guidance and echoed by Artist Dental Lab’s own product architecture for E.max crowns and full-contour multilayer zirconia.
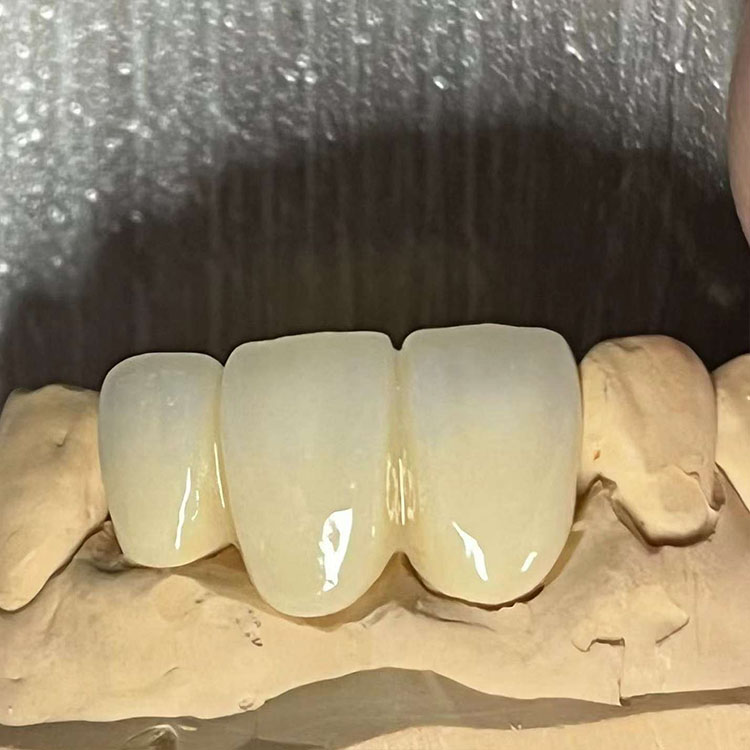
Tiny contamination. Big consequences.
Ivoclar’s guidance makes another point that does not get enough airtime: after intraoral try-in, the restoration should be cleaned thoroughly, but renewed etching or renewed sandblasting is not automatically required and can even damage the surface if people start improvising. So when clinicians “freshen up” the intaglio without a real protocol, they may be solving nothing and adding risk. Who taught that habit, exactly?
My blunt opinion is this: the industry spends too much time arguing about whether lithium disilicate vs zirconia is “better” and not enough time asking whether the case data was good enough to support the chosen material in the first place. The site’s own recent piece on coordinating anterior and posterior materials in full-mouth rehabilitation gets this mostly right by steering posterior load toward zirconia more often and reserving more optical demand for E.max or layered options where the esthetic payoff is real.
And for veneers, the split is even more revealing. Full E.max veneers are positioned around monolithic lithium disilicate, predictable fit, and adhesive bonding, while layered E.max veneers are positioned around a lithium disilicate core plus porcelain layering for more depth, halo, and texture. In other words, even within the E.max family, surface treatment may stay in the same chemical lane, but the risk of variability rises as layering and esthetic ambition rise.
Data hurts.
The older evidence base reviewed by NCBI Bookshelf reported 5-year survival rates of 91.2% for densely sintered zirconia crowns and 96.6% for leucite/lithium-disilicate reinforced glass crowns, with posterior zirconia and anterior zirconia performing differently and older veneered zirconia carrying more chipping and retention baggage than sales teams liked to admit. That historical baggage still shapes how many dentists talk about zirconia today.
But the more recent picture is less sentimental and more interesting. A 2025 PubMed-indexed retrospective cohort study reported a 5-year cumulative survival rate of 94.0% for zirconia and 89.0% for lithium disilicate, with the difference not reaching statistical significance, which is a polite academic way of saying both materials can work, but zirconia keeps looking mechanically harder to kill in tougher indications. Surprised? You should not be.
And when zirconia is used in a disciplined framework-based design, the numbers can get even more stubborn. A 2022 five-year clinical evaluation of posterior zirconia fixed dental prostheses veneered with milled lithium disilicate reported a 100% survival rate at 60 months for the evaluated cases, which is a useful reminder that “zirconia vs lithium disilicate” is sometimes the wrong question; sometimes the better question is how they are combined and where the interfaces sit.
This is where clinicians get ideological.
E.max usually rewards a cleaner adhesive story because the glass-ceramic surface can be etched and silanated in a familiar way, while zirconia can sometimes live with conventional cementation when prep retention is strong, yet becomes far less forgiving when the operator assumes retention geometry will rescue a weak or contaminated bonding surface. Why gamble on prep geometry when chemistry is already telling you what it needs?
That is why I like how Artist Dental Lab separates zirconia veneer cases with higher functional demands from E.max crown workflows for esthetic zones. The site is quietly admitting what many labs know but say too softly: not every pretty case should be E.max, and not every durable case should be zirconia. The surface treatment decision starts the moment the material is chosen.
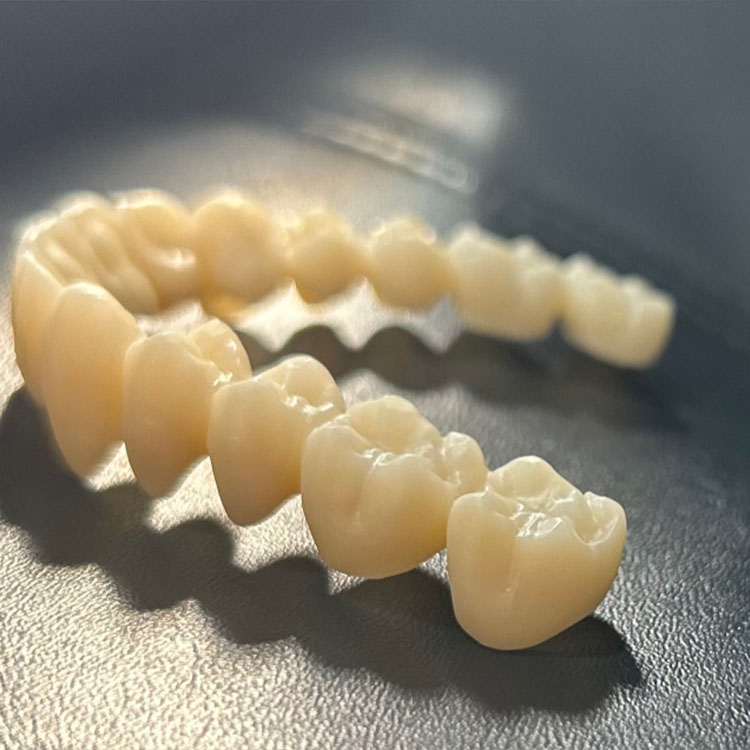
E.max surface treatment means conditioning a lithium disilicate glass-ceramic by creating an etched internal surface and then applying silane so resin cement can couple to it, while zirconia surface treatment means roughening an oxide ceramic and applying an MDP-containing primer because there is no glass phase to etch or silanate in the same way. That is the short answer, and honestly, it is the answer that matters most.
Bonding E.max crowns correctly means following a lithium disilicate protocol that conditions the intaglio with hydrofluoric acid or an approved etch-prime alternative, applies silane chemistry, and then uses the clinician’s selected resin-based cementation workflow according to preparation design, thickness, and esthetic demands. Miss the surface prep, and the rest of the appointment becomes damage control.
The best primer for zirconia is an MDP-containing primer, because zirconium oxide does not contain the glass particles that silane relies on, so the bond has to be built around oxide-compatible chemistry after controlled surface roughening rather than around a glass-ceramic playbook. If someone sells you zirconia as “just like E.max but stronger,” they are selling comfort, not chemistry.
Lithium disilicate vs zirconia is really a case-selection decision in which lithium disilicate often shines in esthetic zones and bonded workflows, while zirconia often earns its keep in higher-load, posterior, implant-supported, or function-heavy situations where mechanical reliability and chipping resistance matter more than squeezing out the last bit of translucency. The wrong answer is pretending there is one universal winner.
Be blunt with the case.
If the restoration is glass-ceramic, treat it like glass-ceramic. If it is zirconia, stop running an E.max script on a different substrate. That sounds obvious, but a shocking amount of remake cost still comes from teams who confuse premium branding with interchangeable bonding chemistry.
For labs and clinics building a cleaner workflow, I would start by matching the case to the right category on the site before the prescription is written: E.max crowns for esthetic-zone control, full-contour multilayer zirconia for posterior function, layered zirconia crowns for smile-zone strength plus characterization, and full E.max veneers or layered E.max veneers when the cosmetic target justifies it. Then send the case properly through Artist Dental Lab’s contact page with shade, stump shade, photos, margin notes, and occlusal guidance instead of hoping the lab will read minds. That is not luxury. That is basic discipline.