


E.max, zirconia, and feldspathic veneers are not interchangeable “premium” options. They are different risk profiles. This guide explains when each anterior veneer material makes sense, when it fails, and why case selection matters more than brand loyalty.
The better question is nastier, more clinical, and less marketable: what can this specific tooth tolerate after reduction, stump shade, occlusion, enamel remaining, smile line, and patient expectations are all counted honestly? That is where anterior veneers stop being cosmetic catalog items and start becoming a risk-management exercise.
I’ll be blunt. I do not trust material loyalty in anterior veneers. I trust enamel. I trust photos. I trust stump shade. I trust a dentist who sends bite notes, retracted images, face photos, preparation design, and a real esthetic target instead of asking the lab to “make it natural.” What does that even mean?
E.max veneers, zirconia veneers, and feldspathic veneers can all be defensible. They can also all be the wrong call. The difference is not romance; it is indication discipline.
That is why I like treating Artist Dental Lab’s own product structure as a useful internal map. Their E.max veneer workflow is positioned around lithium disilicate, fit, strength, translucency, and predictable cosmetic outcomes, while the layered E.max veneer option pushes depth, vitality, incisal effects, and premium characterization. Their feldspathic veneer page leans into enamel-like translucency and micro-texture, and the zirconia veneer page is clearly framed for durability-heavy cosmetic cases. That is not random navigation; it is a case-selection ladder.
Here is the number that should calm everyone down.
A 2025 PubMed-indexed meta-analysis reported pooled survival rates at 10.4 years of 96.13% for feldspathic veneers and 96.81% for lithium disilicate veneers, with zirconia showing 100% survival at 2.6 years but without long-term zirconia veneer data. That is the uncomfortable part: long-term glass-ceramic evidence is mature; zirconia veneer evidence is still young. The survival and complication-rate meta-analysis is worth reading before anyone declares a universal winner.
If a prep stays mostly in enamel, the material has a better shot. A 2025 retrospective study of 672 veneers followed for 1 to 15 years reported 99% survival for veneers bonded entirely to enamel versus 94% when bonded to mixed enamel and dentin. That is not a small footnote; that is the central argument. The dentin exposure and tooth vitality study makes a boring truth hard to ignore: aggressive preparation can make even a beautiful material look dumb.
And then there is the street-level problem nobody in glossy veneer advertising wants to own. The American Dental Association warned on May 14, 2024, that unlicensed “veneer technician” services can create risks including infection, nerve damage, choking hazards, and irreversible harm; the ADA statement on veneer technicians is a reminder that veneers are not nail extensions for teeth. They are irreversible dentistry when tooth structure is altered.
E.max veneers are usually lithium disilicate restorations, often discussed through the IPS e.max system, where the manufacturer lists IPS e.max CAD at 530 MPa flexural strength with multiple translucency and shade options. That number does not mean every E.max veneer survives poor preparation, bad bonding, or parafunction, but it explains why lithium disilicate became the practical middle ground for many anterior veneer material selection decisions.
For routine porcelain veneers for front teeth, I usually think of E.max first when the case needs a balance of bondability, strength, translucency, shade control, and scalable lab repeatability. It is not the most poetic ceramic. It is not always the most enamel-like. But in a six-to-ten-unit anterior case where the dentist wants consistency from canine to canine, poetic is not always your friend.
The full E.max veneer option makes sense when you want lower workflow variance, especially across multiple anterior units where value control and repeatable contour matter more than hand-built incisal drama. The deeper internal read, Full E.max Veneers vs Layered E.max Veneers, is useful because it says the quiet part clearly: full and layered E.max are not the same clinical bet.
Use E.max veneers when the patient has moderate shade needs, stable occlusion, decent enamel preservation, and a smile design that demands repeatability more than handmade translucency theatre.
That sounds conservative. Good.
In a multi-unit smile makeover, conservative thinking saves money. It saves remakes. It saves awkward try-in conversations where everyone stares at tooth #8 and pretends the value is “almost there.”
Feldspathic porcelain is dangerous because it can be gorgeous.
I mean that. Its strength is also how clinicians get seduced. Feldspathic veneers can create delicate enamel-like translucency, incisal halo, surface texture, and subtle value shifts that make a single central incisor or minimal-prep smile case look less manufactured. The problem is that feldspathic is not a forgiveness machine.
It wants enamel. It wants conservative preparation. It wants a calm bite. It wants a ceramist who can actually layer porcelain, not just say “custom” on a brochure. It also wants a dentist who understands that a thin, translucent ceramic cannot magically mask every dark stump without either overbuilding, over-opacifying, or overpromising.
Artist Dental Lab’s hand-layered feldspathic veneer indications are aligned with that narrow, high-end lane: minimal-prep cosmetic cases, complex shade blending, delicate incisal effects, and high-end smile design. That is where feldspathic belongs. Not everywhere. Not automatically. Not because a patient brought in a celebrity photo with ring-light teeth.
Choose feldspathic veneers when enamel is abundant, shade change is modest, the preparation is conservative, and the esthetic demand is extreme enough to justify the technique sensitivity.
A hard truth: many cases sold as “feldspathic cases” are actually poor diagnostic cases wearing luxury language.
Zirconia veneers have a place.
A narrow place.
Modern translucent zirconia is far better than the dead-white blocks people still joke about, and zirconia can make sense in functional cosmetic cases where fracture resistance matters more than maximum glass-ceramic translucency. But when someone casually says zirconia is “better” for anterior veneers, I want to see the bonding protocol, surface treatment, restoration thickness, tooth shade, smile line, and occlusion before I take that seriously.
A 2025 randomized controlled trial on zirconia veneers bonded with MDP-containing polymeric adhesives supported the clinical relevance of polymeric bonding systems for zirconia veneer performance, but the same evidence space is still younger than lithium disilicate and feldspathic veneer survival research. The zirconia veneer bonding trial is promising, not a license to treat zirconia as the new default for every anterior veneer.
This is where the zirconia veneer workflow fits best: high-strength cosmetic cases, stronger functional demands, and situations where durability gets priority over maximum natural translucency. If the patient is a bruxer, edge-to-edge, or functionally risky, zirconia deserves a look. If the patient has thin enamel, high esthetic expectations, and a bright smile line, I slow down.
Use zirconia veneers selectively for higher-risk functional cases, masking-heavy edge cases, or patients where fracture resistance is a stronger clinical priority than maximum enamel mimicry.
Would I use zirconia for every anterior veneer case? No. And I would be suspicious of anyone who says yes.
| Case Factor | E.max Veneers | Zirconia Veneers | Feldspathic Veneers |
|---|---|---|---|
| Best overall use | Everyday anterior veneers needing strength, translucency, and predictable workflow | Functional cosmetic cases needing added fracture resistance | Minimal-prep, high-end esthetic cases needing enamel-like optics |
| Esthetic ceiling | High, especially with layered or cut-back designs | Improving, but still less glass-like in many thin anterior cases | Very high in elite hands |
| Strength profile | Strong lithium disilicate; IPS e.max CAD marketed at 530 MPa flexural strength | High-strength ceramic family; depends heavily on bonding and surface treatment | More technique-sensitive and less forgiving |
| Bonding confidence | Strong adhesive history when enamel is preserved | More protocol-sensitive; MDP systems matter | Excellent when bonded to enamel |
| Dark stump control | Good with lower-translucency or monolithic strategies | Useful in masking-heavy cases, but esthetics must be managed carefully | Weak if translucency becomes a liability |
| Best preparation style | Conservative to standard veneer prep with clear margins | Case-dependent; avoid pretending strength fixes diagnosis | Minimal-prep or enamel-dominant preparation |
| Main failure risk | Poor prep data, shade drift, bonding errors, occlusion | Bonding protocol errors, opacity mismatch, overuse in high-esthetic cases | Fracture, chipping, over-translucency, weak masking |
| My blunt verdict | Best default for many anterior veneers | Best selective tool for riskier function | Best beauty tool when the case truly deserves it |
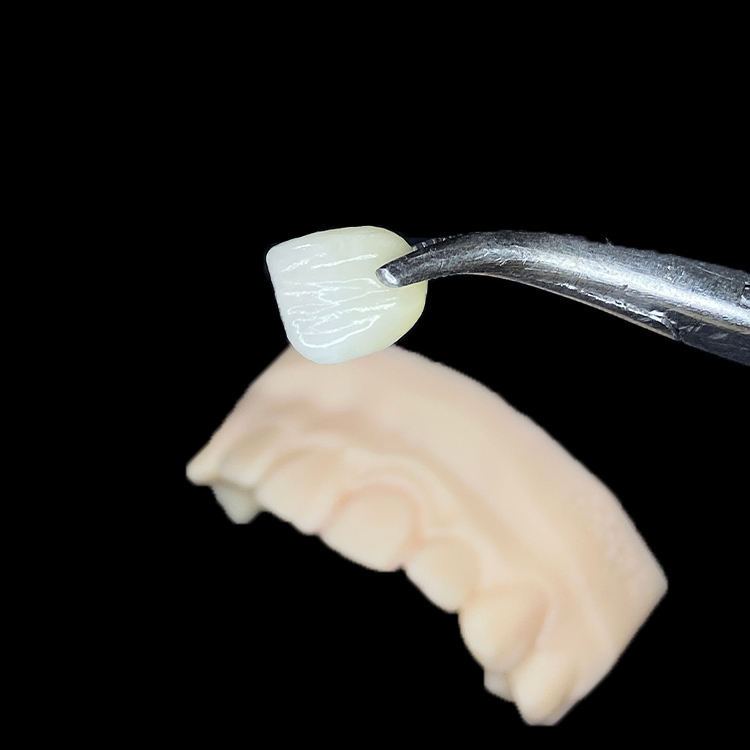
Dark stumps punish.
If the underlying tooth is A4-dark, endodontically shifted, tetracycline-banded, or heavily discolored, the veneer material has to do more than look pretty on a model. It must control value, opacity, cement shade, ceramic thickness, and the visual transition at the margin.
This is where I often choose lower-translucency E.max before feldspathic. Not because feldspathic is inferior, but because a translucent masterpiece over a dark stump can become a gray disappointment. The internal guide on which veneer material works best for dark stump cases gets this right: masking is not a beauty preference; it is an optical problem with biological costs.
And here is the uncomfortable tradeoff. More opacity can hide darkness, but too much opacity kills vitality. More reduction can create space, but more reduction may sacrifice enamel. More ceramic can correct color, but overcontour can inflame tissue and ruin emergence. Who exactly benefits when we pretend this is simple?
Choose E.max veneers when the case is routine-to-premium, the stump shade is manageable, the smile design spans multiple units, and the clinician wants a strong balance between esthetics and repeatability. For many anterior veneers, this is the safest first conversation.
Choose layered E.max when the case has high esthetic demand, excellent records, good preparation space, clear shade communication, and a patient who genuinely needs refined incisal effects. Layering without data is not artistry. It is gambling.
Choose feldspathic veneers when the preparation is conservative, enamel bonding is strong, shade change is modest, and the patient’s main demand is natural light behavior rather than masking or brute strength.
Choose zirconia veneers when functional risk, fracture resistance, or masking needs justify moving away from classic glass-ceramic thinking. But do not call it the most natural option by default. That is sales talk.
The best material for anterior veneers is the ceramic that matches the tooth’s enamel remaining, stump shade, preparation design, occlusion, esthetic target, and bonding risk; in many everyday cosmetic cases that means E.max, while feldspathic wins selective beauty cases and zirconia fits higher-strength functional cases. After that, the real decision depends on records.
For a broad six-to-ten-unit case, I usually start with E.max veneers. For a minimal-prep, enamel-rich, high-esthetic case, I seriously consider feldspathic. For functional risk, zirconia enters the conversation.
E.max veneers are often better than zirconia veneers for anterior cases that need reliable translucency, proven long-term glass-ceramic evidence, adhesive bonding predictability, and natural shade integration; zirconia may be better when fracture resistance, functional demand, or masking risk outweighs the need for maximum enamel-like light transmission. The winner is case-specific.
The lazy answer is “E.max looks better, zirconia is stronger.” The better answer is that E.max vs zirconia veneers is a surface-treatment, optical, bonding, and preparation-design decision.
Feldspathic veneers should be used when the clinical case has abundant enamel, conservative preparation, stable occlusion, limited shade change, and a high demand for hand-layered enamel-like translucency, incisal effects, and micro-texture that justify the added technique sensitivity. They are premium tools, not universal solutions.
I like feldspathic most when the goal is not just “white teeth,” but believable anterior character. That means the case must deserve it.
Zirconia veneers can look natural on front teeth when the case is designed with proper thickness, translucency selection, shade communication, surface finishing, bonding protocol, and realistic esthetic expectations; however, they are usually selected more for durability and masking control than for the highest possible glass-ceramic enamel mimicry. That distinction matters.
Zirconia is not ugly. Badly indicated zirconia is ugly. There is a difference.
To choose veneer material for dark stump cases, first diagnose the severity of discoloration, then balance ceramic opacity, thickness, cement shade, preparation depth, and enamel preservation; lower-translucency lithium disilicate often becomes the practical choice, while feldspathic is selective and zirconia remains a niche option for severe masking or function. This is planning, not branding.
Dark stumps are where “natural translucency” can become the enemy. The goal is controlled brightness, not blind transparency.
The smartest anterior veneer material selection is not E.max, zirconia, or feldspathic in isolation. It is a case file that tells the truth: stump shade, enamel left, bite risk, prep design, reduction, desired value, photo references, and patient expectations.
Send the lab better evidence.
If you are planning anterior veneers and want a material recommendation that does not hide behind generic sales language, start with Artist Dental Lab’s E.max veneer, layered E.max veneer, feldspathic veneer, and zirconia veneer workflows, then submit a trial case with full photos, stump shade, STL files, occlusion notes, and the esthetic target you actually want.
Do that, and the material decision gets easier. More importantly, the remake risk gets smaller.